Introduction
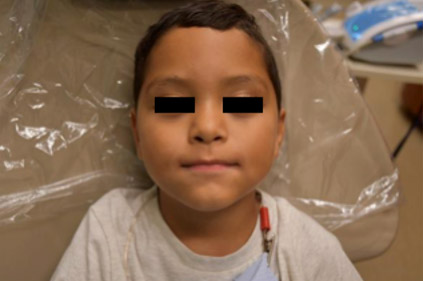
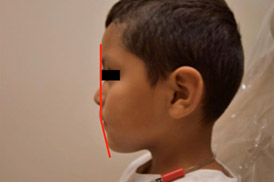
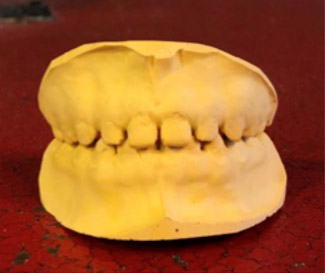
- 6 year old Hispanic male presented to the San Jose Clinic in Houston, TX on 8/18/18 for a comprehensive examination. (Fig 1)
Medical History
- Patient reports a history of seasonal asthma “When its cold” and uses an albuterol inhaler when indicated.
- Patient reports no hospitalizations
- Patient reports no other significant medical history
- Patient weighed 20kg on day of examination
- Patient’s mother reports brushing once a day in the morning
- Patient uses Colgate fluoridated toothpaste
- Patient drinks two cups of juice a day
- Patient snacks throughout the day on “fruits and crackers”
- Patient rarely drinks water and if he does its from the bottle (not fluoridated)
Dental History
- Patients mom reports only going to the dentist “for emergencies”
- Patients mom reports that finances are an issue, she is uninsured, and she cannot afford to take her child to the dentist regularly
- Patients mom reports that her child “fell off his bike a few years ago and broke his front teeth”
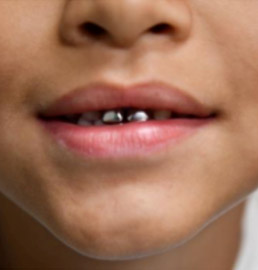
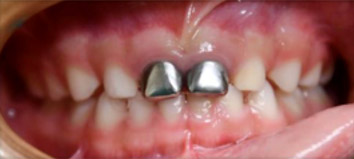
- Mom reports that a dentist put “silver caps” on the two front teeth to protect them, her child was very fearful and anxious throughout the procedure.
Clinical Examination
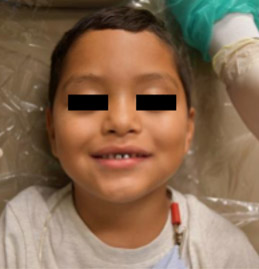
- Symmetrical Profile Noted
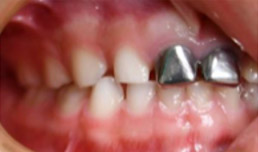
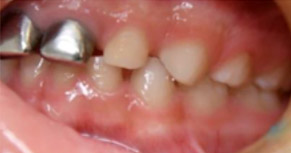
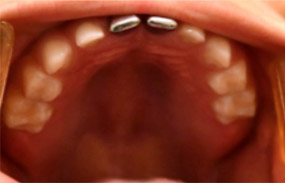
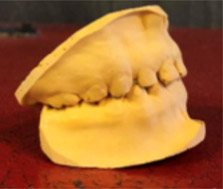
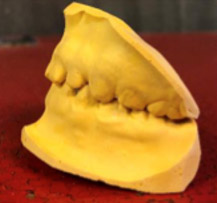
- SSC’s noted on E&F (Fig 2 and Fig 3)
- Adequate maxillary and mandibular spacing
- 2 mm overjet
- 25% overbite
- Prominent primate spaces
- Gingiva within normal limits
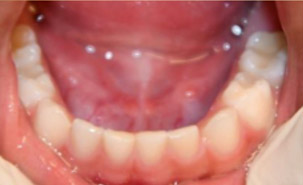
- Moderate plaque (Fig 4)
- Right/Left side: Mesial Step (Fig 5 and Fig 6)
- Generalized attrition noted
- No mobility on any teeth
- Full primary dentition noted (Fig 7 and Fig 8)
- Slight skeletal class II
- Convex facial profile (Fig 9)
Radiographic Examination
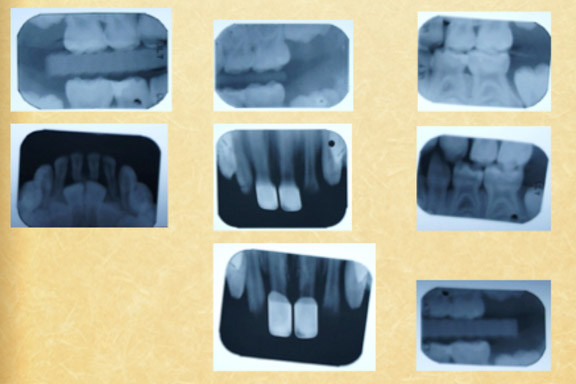
- Bitewings and occlusal radiographs were ordered
- This is due to interproximal contact in the posterior
- Periapical radiograph was taken of #K in order to evaluate radiolucency.
Radiographic Findings
- Fig 10
- Distal caries noted on #B, Normal Growth of #3 & #30, Previous composite restoration on #S (Fig11)
- Normal Growth of #14 & #19, Previous composite restoration on #L, Questionable radiolucency on #K (Fig12)
Treatment
- Prophy performed and impression taken to better visualize the primary dentition
- Fluoride varnish was applied after (Fig 13, Fig14, Fig15)
Growth and Development
- This patient is 6 years old and showed no signs of mobility on any of his primary incisors.
- This patient is slightly dentally delayed and we told his mother that he should expect to lose some of his front teeth within the next year.
Space Analysis
- Tanaka-Johnson space analysis will be carried out once the permanent four mandibular incisors are present.
- Tanaka-Johnson mixed dentition analysis allows one to estimate the space available in an arch for the permanent teeth to erupt.
- This patient has adequate spacing with no crowding on the maxillary and mandibular arch.
- Monitoring is necessary as growth continues
Treatment Plan
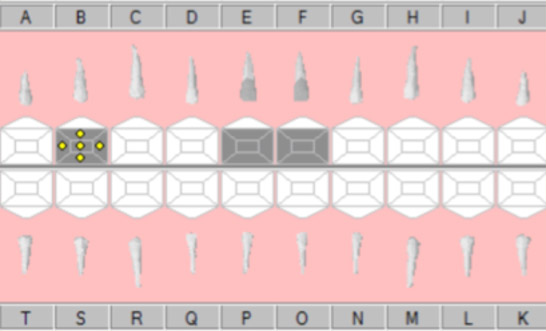
- #B – SSC
- #K – Monitor
- Fig 16
Treatment Outcomes
- Given this patients caries risk, is it important to remove any active decay in his mouth and get him to a point where all he has to worry about is maintenance.
- It is important to establish a series of good habits for this patient, encouraging better home health practices as well as nutritional counseling.
- Desensitization is also crucial. We need to get this patient used to coming to the dentist in order to gain his trust.
Patient Management
- Maximum amount of 2% lidocaine with 1:100k epi (1.8ml)
- 20kg patient
- Total maximum dose: 88mg
- Total mg/carpule: 36mg
- 2.4 carpules maximum for a 20kg patient
- We will start by doing the simple procedures (prophy/exam) and work our way to the more complex procedures (SSC).
- Tell-show-do is very important for this patient, he was very anxious about the new environment and everything must be explained.
- Distraction is also a possible way to help this patient get through this procedure. This patient was is a fan of “Paw Patrol” and watching this show during the procedure could help him get through it.
- Voice control/inflection/voice modulation if you have started the procedure and he starts to act up mid way throughout.
- Nitrous Oxide is also a possible way to manage an anxious patient.
- Dental jargon is commonplace amongst dental providers. For that reason it is important to speak in a language that children and parents can understand.
- This will help facilitate understanding between the patient, parent and the provider.
Patient Education
- Nutritional counseling
- The American Academy of Pediatric Dentistry (AAPD) recommends only 1 cup (4-6 ounces) of juice once a day
- Avoid fermentable carbohydrates such as refined sugar
- Cut the snacking and limit food to meal time
- Oral Health Habits
- Have mother help her son with brushing until he has the dexterity to tie his own shoes
- Encourage the mother to have her child brush twice a day but if he is to brush once, make sure it is at night
- Encourage flossing since he has proximal contact in the posterior
- Explain the etiology of caries
- Provide patient with floss, toothbrush and Colgate toothpaste
- Instruct patient to wash mouth out after the use of his inhaler
Preventative Plan
Recall schedule
- 3 month recall with clinical exam, prophy and fluoride. Bitewing radiographs every 6 months.
- It might be difficult to make sure that this patient comes in for his recalls due to his previous dental history. It is imperative to establish rapport with the parent and the child and encourage the establishment of a dental home.
Fluoride Treatment
- Regular fluoride varnish is essential at 3month recall examination.
- Brushing twice a day with fluoridated toothpaste.
- Talking to patients who cannot afford dental visits is a challenge.
- It is important to have a list of convenient low cost/free clinics that will be able to provide dental services to low income households.
- These patients and their parents need to realize the importance of the establishment of a dental home for their recalls.
- Daily maintenance with fluoride toothpaste and fluoridated mouthwash is critical to preventing caries from forming and progressing.
- 3 month recalls due to this patients caries risk will help to catch caries before they progress. Fluoride vanish can be applied during each visit.
- Anticipatory guidance will also help
- Additionally, seeing a dentist regularly will help find malocclusions and other anomalies early which will save them money in the long run.
Uninsured Population
- For the uninsured population, it can be difficult to maintain a regular oral health maintenance schedule.
- This is a barrier to care
- Insurance companies usually cover two visits a year and this might not be enough for some patients that are at a higher risk for dental caries.
Difficulties
- San Jose Clinic is one of the safety net clinics in Houston, Texas.
- All of the materials and equipment are donated which made it difficult to gather records due to lack of equipment.
- Cheek retractors were badly damaged and intraoral mirrors were scarce, film radiography is used which makes presentation of the radiographic findings difficult.
Importance of Safety Net Clinics
- San Jose Clinic and other safety net clinics in the Houston area are imperative to serving the disadvantaged population.
- This clinic works to help the uninsured and low income population in the area.
- If it wasn’t for clinics like these, a lot of children would not be able to receive any form of dental care.
Safety Net Clinics
- The generous volunteers make this clinic happen and provide optimal dental care for the disadvantaged population.
- The donations of time, equipment and material are imperative for the sustainability of this clinic.
- If it was not for these various safety net clinics, these patients would not have a location to receive care.
Socioeconomic Factors
- According to the CDC, Hispanics have the poorest oral health of any racial and ethnic group in the United States.
- The economic factors that often relate to poor oral health include access to health services and the individuals ability to get and keep dental insurance.
- Various organizations such as the Hispanic Dental Association work towards breaking down these barriers.
Cultural Factors
- Social factors can contribute to the oral health of this patient as well as the Hispanic community as a whole.
- Lifestyle behaviors such as familial tobacco use, frequency of alcohol use and poor dietary choices can affect the overall health of this child.
- A lot of families that struggle with income tend to prioritize other health issues over their oral health.
- Education is the cornerstone of this process.
- The language barrier is also an important consideration.
- It is important to have a provider that can speak the same language as the parent or have an interpreter that can make appropriate translations.
Conclusion
- Through cases like this, we can raise awareness of various programs that are aimed at helping children receive dental care despite financial barriers.
- If it was not for organizations like these, these patients would never receive the care they need
- There are various outlets for these patients that we, as future dental providers need to be aware of and promote.
- Companies such as Colgate help to promote early dental visits as essential to the overall health of the child.
Acknowledgments and Consents
- A big thank you to the staff at San Jose Clinic for their continued support of UTSD dental students.
- Proper consent for this case presentation was carefully documented in the clinic records.
References
- Dean, Jeffrey A., et al. McDonald and Avery Dentistry for the Child and Adolescent. Elsevier, 2011.
- Disparities. (n.d.). Retrieved from https:// www.healthypeople.gov/2020/about/foundation-health-measures/Disparities
- Early Dental Visits Essential for Children | Colgate® Oral Care. (n.d.). Retrieved from https://www.colgate.com/en-us/oral-health/basics/dental-visits/ada-02-early-dental-visits-essential-childrens-health
- Koch Göran, et al. Pediatric Dentistry: a Clinical Approach. John Wiley & Sons, Ltd, 2017.
- Nowak, Arthur J., and Paul S. Casamassimo. The Handbook of Pediatric Dentistry. American Academy of Pediatric Dentistry, 2018.
- Office of the Surgeon General (US). (1970, January 01). National Call To Action To Promote Oral Health. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK47472/
- Oral Health. (2018, March 15). Retrieved from https://www.cdc.gov/oralhealth/oral_health_disparities/index.htm
- OSG. (n.d.). Reports of the Surgeon General, U.S. Public Health Service. Retrieved from https://www.surgeongeneral.gov/library/reports/
- Fig. 1
- Fig. 2
- Fig. 3
- Fig. 4
- Fig. 5
- Fig. 6
- Fig. 7
- Fig. 8
- Fig. 9
- Fig. 10
- Fig. 11
- Fig. 12
- Fig. 13
- Fig. 14
- Fig. 15
- Fig. 16


:sharpen(level=0):output(format=jpeg)/up/2023/05/Nick-Rodriguez-3.jpg)
:sharpen(level=0):output(format=jpeg)/up/2019/08/Raising-Awareness-for-Safety-Net-Dental-Clinics-A-Case-Studyjpg.jpg)