Introduction:
The first two parts of this update on the recent literature examining the relationship of diabetes mellitus (DM) and oral disease focused on DM and periodontal disease and endodontic complications (part 1) and tooth loss and implant complications (part 2). This third part of the review will examine recent literature on other complications of DM, and identification of pre-diabetes (pre-DM) and DM in the dental office. Lastly, a developing area of investigation will be reviewed: the effect of preventive dental care/periodontal care on general health outcomes, including use of specific services such as visits to the emergency department and hospitalizations, as well the medical costs associated with these services.
It is important to emphasize that identification of dysglycemia (DM and pre-DM) in the dental office, and findings concerning the relationship of preventive dental care to health outcomes, are still developing areas of investigation. The former represents an aspect of dental patient care that is not generally considered within the scope of dental practice but has important implications for the oral health and general health of patients. In the latter case, this represents a potentially very important benefit of preventive care that has broad implications for closer alignment of dental and medical reimbursement.
It is clear from the review of the past and recent literature that regardless of the age at the time of diagnosis, once the diagnosis of DM is made, oral health care should become a routine part of the patient management. This includes both regular professional care and a special emphasis on self-care. Topics covered in this essay emphasize the growing importance of interprofessional care for persons with DM.
Other Oral Complications of DM:
As noted in the first part of this series, in addition to the well-recognized oral complications of DM such as periodontal disease, endodontic complications, tooth loss and implant complications, other oral complications must be considered. These include, but are not limited to, oral cancer, burning mouth syndrome and Candida infection.
The recent literature has addressed some of these other complications. A systematic review with a meta-analysis of the relationship between DM and oral cancer included 52 studies.1Ramos-Garcia P, et al. Diabetes mellitus and oral cancer/oral potentially malignant disorders: A systematic review and meta-analysis. Oral Dis. 2021;27(3):404-21 https://www.ncbi.nlm.nih.gov/pubmed/31994293. The analysis determined that there was an increased risk of oral cancer in persons with DM, with an odds ratio of 1.41 (41% higher chance of developing oral cancer). They also concluded that the mortality rate was higher for persons with DM and oral cancer as compared to oral cancer patients without DM. However, it is important to note that not all studies agree with these conclusions. A study from Hyderabad India observed that as compared to persons without DM, a lower rate of oral cancer was seen in patients with DM.2Mekala MR, et al. Association of diabetes with oral cancer - an enigmatic correlation. Asian Pac J Cancer Prev. 2020;21(3):809-14 https://www.ncbi.nlm.nih.gov/pubmed/32212811. This emphasizes the importance of considering all variables in such studies, including cultural habits such as use of chewing betel nut preparations, as well as tobacco use, and use of prescription medications.
An interesting report on burning mouth syndrome3Bookout GP, et al. Burning Mouth Syndrome. StatPearls. Treasure Island (FL)2021. reminds us that many oral disorders associated with DM are not unique to DM. These authors classified burning mouth syndrome into 3 types:
- Type 1: no symptoms upon awakening, but symptoms worsen during the day. Symptoms at night can vary. This type is associated with DM and nutritional deficiencies.
- Type 2: long-standing anxiety is the underlying association. Symptoms are present when awake, but generally not at night.
- Type 3: occasional daytime symptoms but extended periods without symptoms are observed. The underlying cause is believed to be a food allergy.
Of note, the recent literature contains an emphasis on the relationship of oral Candida infection in the context of DM. Candida is a normal component of the oral microflora, and in health does not manifest clinically. An increase in clinical Candida infection of the oral cavity is seen in association with DM. Recent studies have examined different aspects of the characteristics of oral Candida species in persons with DM.
There are several species of Candida that have been identified in the oral cavity, but the predominant species of fungus in the mouth is Candida albicans. A study of the species of oral Candida in persons with and without DM indicated that there was a higher carriage rate (greater density of fungal organisms) in the mouths of persons with DM. Candida albicans was the predominant species4Patel PN, et al. Oral candidal speciation, virulence and antifungal susceptibility in type 2 diabetes mellitus. Diabetes Res Clin Pract. 2017;125:10-9 https://www.ncbi.nlm.nih.gov/pubmed/28131069. Less common species such as Candida lusitaniae and Candida lipolytica were also identified. Of importance, the non-albicans Candida species were detected more often in persons with DM. There was also a suggestion that susceptibility to the anti-fungal agent fluconazole was reduced in species isolates from persons with DM.
A subsequent study examined Candida infection in metabolically poorly controlled, moderately-well controlled, controlled, and non-DM individuals. The frequency and carriage rate of Candida was highest in the poorly controlled individuals. The major fungal species in the mouth was Candida albicans, and in this study the isolates from individuals with poorly controlled DM demonstrated greater resistance to fluconazole as compared to the organisms isolated from the healthy control subjects5Bhuyan L, et al. Candida species diversity in oral cavity of type 2 diabetic patients and their In vitro antifungal susceptibility. Contemp Clin Dent. 2018;9(Suppl 1):S83-S8 https://www.ncbi.nlm.nih.gov/pubmed/29962770.. The authors also raised concerns about other Candida species colonizing the oral cavity in persons with DM. A subsequent study examined the pathogenicity of Candida albicans isolated from the mouths of persons with DM.6Nouraei H, et al. Potential pathogenicity of candida species isolated from oral cavity of patients with diabetes mellitus. Biomed Res Int. 2021;2021:9982744 https://www.ncbi.nlm.nih.gov/pubmed/34136578. A total of 108 Candida isolates were studied, including 75 identified as Candida albicans and 33 as non-Candida albicans. Enzyme activity was studied, and Candida albicans isolates demonstrated greater activity than the non-Candida albicans isolates. The authors concluded that the dominant fungal species in the oral cavity of persons with DM demonstrated high levels of enzyme activity, contributing to pathogenicity.
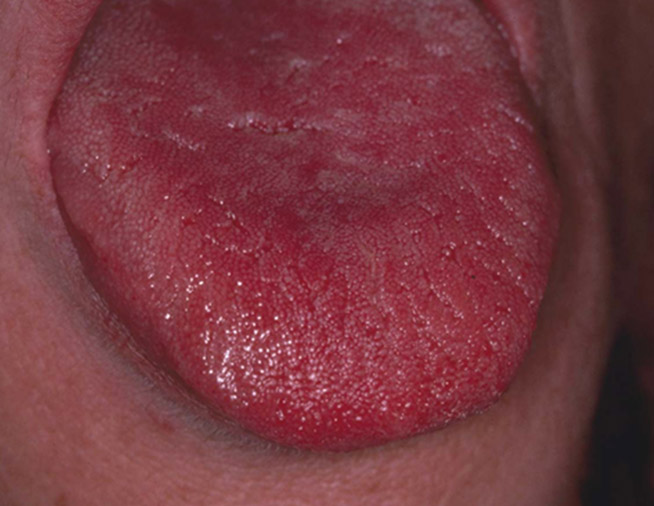
In terms of the effect on patients, a review of the Candida carriage rate in denture patients with and without DM included 9 studies.7Javed F, et al. Oral Candida carriage and species prevalence in denture stomatitis patients with and without diabetes. J Biol Regul Homeost Agents. 2017;31(2):343-6 https://www.ncbi.nlm.nih.gov/pubmed/28685534. The prevalence of Candida-associated denture stomatitis was higher among patients with DM as compared to patients without DM. Candida albicans was the predominant species. The relationship of several risk factors and health outcomes in relationship to the presence of Candida in the oral cavity has also been studied. Patients on hemodialysis were evaluated. Recall that hemodialysis is needed when a person is in kidney failure, and chronic kidney disease and kidney failure are often a complication of DM. They observed that oral Candida infection was associated with DM (p=0.001) as well as age and cardiovascular disease. In these hemodialysis patients, oral Candida infection was also associated with higher concentrations of systemic markers of inflammation. While the authors associated oral Candida infection with the development of atherosclerosis in these patients, the complex interaction of risk factors and clinical conditions makes it impossible to tease out cause and effect8Yeter HH, et al. Oral candida colonization as a risk factor for chronic inflammation and atherosclerosis in hemodialysis patients. Ther Apher Dial. 2019;23(6):542-9 https://www.ncbi.nlm.nih.gov/pubmed/30895718.. Nevertheless, these data indicate that oral candidiasis can identify a person who is at risk for an underlying systemic disorder, or a patient with a previously diagnosed disease who is not well managed. Awareness of the multiple presentations of oral candidiasis is essential (Figure 1).
Identification of Dysglycemia (Pre-diabetes and Diabetes) in Clinical Dental Settings:
DM as the only recognized systemic risk factor for periodontal disease, and interest has been focused on how dental clinicians can improve care of their patients with DM. Recall that the prevalence of DM is high. In the United States, 10.5% of the population is estimated to have DM, and 13% of adults have the disease. Prevalence increases with age, and more than a quarter of older adults (65 years and older) have DM. In addition, approximately 21% of persons with DM in the U.S. are unaware of their diagnosis.9Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2020. Further, an estimated 88 million persons 18 years of age and older in the U.S. have pre-DM, and pre-DM is often underdiagnosed and/or untreated. Lastly, the percent of patients diagnosed with DM, but who are not well managed, also represents a health challenge.10Chasens ER, et al. Citizenship and health insurance status predict glycemic management: NHANES data 2007-2016. Prev Med. 2020;139:106180 https://www.ncbi.nlm.nih.gov/pubmed/32593731. As an example, in New York City, nearly 20% of patients with a diagnosis of DM demonstrated an HbA1c level greater than 9%.11Thorpe LE, et al. Change in diabetes prevalence and control among New York City adults: NYC Health and Nutrition Examination Surveys 2004-2014. J Urban Health. 2018;95(6):826-31 https://www.ncbi.nlm.nih.gov/pubmed/29987771.
As a result, studies have examined screening for dysglycemia in dental clinics. These studies have suggested that expansion of the types of services provided by oral health care providers can improve both oral health and general health.
A systematic review of screening procedures for dysglycemia (pre-DM and DM) in dental offices published in 2018 included 10 studies and observed that large percentages of dental patients with dysglycemia were identified. However, various study designs were employed which did not allow for a meta-analysis and estimation of the percent of dental patients who were dysglycemic.12Glurich I, et al. Screening for dysglycaemia in dental primary care practice settings: Systematic review of the evidence. Int Dent J. 2018;68(6):369-77 https://www.ncbi.nlm.nih.gov/pubmed/29740815.
A systematic review with a meta-analysis was published in 2020.13Chinnasamy A, Moodie M. Prevalence of Undiagnosed Diabetes and Prediabetes in the Dental Setting: A Systematic Review and Meta-Analysis. Int J Dent. 2020;2020:2964020 https://www.ncbi.nlm.nih.gov/pubmed/32908510. Nine studies were included, and the percentage who were judged to be at risk for dysglycemia using the point-of-care (chairside) test for serum glucose was 32.5% and using a chairside test for HbA1c was 40.1%. They also estimated the portion for the entire population at risk for undiagnosed type 2 DM and pre-DM, which were 11.2% and 47.4%, respectively.
Another systematic review published in 2020 included 9 studies and reported identification of both pre-DM and DM.14Yonel Z, et al. Use of dental practices for the identification of adults with undiagnosed type 2 diabetes mellitus or non-diabetic hyperglycaemia: A systematic review. Diabet Med. 2020;37(9):1443-53 https://www.ncbi.nlm.nih.gov/pubmed/32426909. They observed ranges of identification of pre-DM (23% - 45%) and DM (1.7% - 24%). These authors however, raised important issues related to this activity in the dental office, mainly clinical effectiveness, and cost effectiveness. They also observed that these studies generally approached screening as a two-step process: the first is deciding which patients should be screened (Step 1), and the second is the actual screening test. (Step 2).
Recent studies help define how this type of activity can be operationalized, and some of these individual reports define the potential impact of this new dental practice activity, and specific aspects of this new practice activity. One approach to determining the potential impact of screening for dysglycemia in the dental office involves analysis of large, existing databases. The National Health and Nutrition Surveys (NHANES) are studies of the health status of a representative group of people in the U.S. This survey is conducted every few years and contains many health and demographic variables and can be used to examine many health care relationships. A study using data from the 2013-2016 NHANES addressed the question of using dental offices to identify previously undiagnosed pre-DM or DM.15Estrich CG, et al. Prediabetes and diabetes screening in dental care settings: NHANES 2013 to 2016. JDR Clin Trans Res. 2019;4(1):76-85 https://www.ncbi.nlm.nih.gov/pubmed/30596147. Data was available for more than 10,000 adults and almost 8% of those surveyed had a dental visit, but not a medical visit, in the prior 12 months. Of this group, nearly one-third were at risk for pre-DM, and the level of HbA1c for more than 15% was in the pre-DM or DM range. The profile of those at greatest risk for pre-DM or DM and had visited a dentist but not a medical provider was at least 45 years of age, who were obese and non-white. Extrapolated to the U.S. population, they estimated that up to 22 million people at risk for pre-DM or DM could be identified in dental offices.
Reports have evaluated different protocols to define screening algorithms to determine who should be tested (Step 1) and then testing identified individuals, generally using a point-of-care test for HbA1c (Step 2). A study from the Netherlands evaluated 204 patients with periodontitis.16Su N, et al. Development and validation of a screening model for diabetes mellitus in patients with periodontitis in dental settings. Clin Oral Investig. 2020;24(11):4089-100 https://www.ncbi.nlm.nih.gov/pubmed/32542584. Here the primary purpose was development of a screening algorithm (Step 1). Of those patients, 17% were classified as DM, and 47% as pre-DM. The parameters that were found to be included in the screening model were age, previous treatment for periodontitis, percent of teeth with mobility, percent with gingival recession, as well as European heritage and level of cholesterol. The creation of receiver-operator curve is a means of displaying the accuracy of the model, with 100% (1.0) being ideal. The percentage area under the curve reflects how close to the ideal is the model, and here it ranged from 0.67 to 0.80. These statistics were judged to be “acceptable”, and the authors concluded that the model could be used to test patients for pre-DM/DM.
Another assessment used an existing research database, here the Atherosclerosis Risk in Communities study. The relationship of previously undiagnosed DM was evaluated in relation to the existing severity of periodontal disease, obesity and edentulism. The intent again was to develop a screening model.17Philips KH, et al. Periodontal disease, undiagnosed diabetes, and body mass index: Implications for diabetes screening by dentists. J Am Dent Assoc. 2021;152(1):25-35 https://www.ncbi.nlm.nih.gov/pubmed/33256949. There were 5.7% of the study participants who had undiagnosed DM. There were associations between the individual variables and DM (severe periodontal disease, odds ratio = 1.78; edentulism, odds ratio = 1.87). Combining obesity with the other 2 variables (periodontal disease, edentulism) further improved identification of participants with DM. It can be concluded that the three variables should alert dental providers to patients at risk for DM.
In addition to using dental clinical parameters (i.e., periodontitis, edentulism) and other clinical personal variables (i.e., obesity) another study considered the addition of a saliva test for the active form of matrix metalloproteinase 8.18Grigoriadis A, et al. Prediabetes/diabetes screening strategy at the periodontal clinic. Clin Exp Dent Res. 2021;7(1):85-92 https://www.ncbi.nlm.nih.gov/pubmed/33300692. This enzyme breaks down collagen and has been associated with destructive periodontal disease. The investigators determined that the addition of the enzyme test to other clinical variables including age, body mass index, the number of teeth present in the mouth and the percent of pockets of 4mm or more could be used as a screening model to identify persons at risk for pre-DM and DM. Of note, they did not include the point-of-care testing for HbA1c here. Instead, they suggested that their model could be used to identify patients who should be referred to a medical provider for further evaluation.
Steps 1 and 2 were combined in a study from Spain.19Montero E, et al. Screening of undiagnosed hyperglycaemia in the dental setting: The DiabetRisk study. A field trial. J Clin Periodontol. 2021;48(3):378-88 https://www.ncbi.nlm.nih.gov/pubmed/33263197. A total of 1,143 patients completed a DM risk questionnaire (the Finnish Diabetes Risk Score or FINDRISC) and received a periodontal examination. A total of 8.5% of patients were diagnosed with dysglycemia as confirmed by a medical provider (2.5% DM, 6.0% pre-DM). They utilized receiver-operator curves and determined the area under the curve. The FINDRISC questionnaire alone provided an AOC of 0.87, adding the findings from the periodontal exam improved the yield (AOC=0.88). Adding the point-of-care HbA1c test to the questionnaire increased the AOC to 0.96. The authors concluded that the use of a screening questionnaire and a point-of-care HbA1c test efficiently identified persons with dysglycemia. A similar approach was reported from the United Kingdom.20Goh G, et al. The prevalence of potentially undiagnosed type II diabetes in patients with chronic periodontitis attending a general dental practice in London - a feasibility study. Br Dent J. 2021;231(3):180-6 https://www.ncbi.nlm.nih.gov/pubmed/34385649. Here patients with periodontitis seen in general dental practices completed the FINDRISC. If the score was elevated, the patient was sent for evaluation by a medical provider. During a one-year period 51 patients were identified with pre-DM or DM, and 40 of these individuals chose to complete the protocol. 79% of patients at risk for dysglycemia were demonstrated to have either pre-DM or DM. The authors concluded that this protocol was effective in identifying dysglycemia in dental patients with periodontitis who were seen in general dental practice.
These studies, while heterogenous in design and setting, suggest that patients with previously undiagnosed dysglycemia (pre-DM and DM) can be identified as part of dental care. These protocols agree that a two-step approach should be used: first a screening phase (Step 1) and then an assessment, usually a point-of-care HbA1c test, which utilizes capillary blood (finger stick; Step 2). The screening phase (Step 1) is intended to increase the percent of patients who are tested (Step 2) who actually have pre-DM or DM (known as ‘true positives’). By so doing, the chance of testing a person who is not dysglycemic is reduced. This saves time and money.
An important issue is the willingness of dental providers to add identification of systemic disease to their practice activities. While earlier literature has indicated a general willingness of dental providers to assume this responsibility, recently published studies have further defined the concerns that accompany the evaluation of dysglycemia in dental settings.
A recent report examined the beliefs of oral health care providers regarding screening for pre-DM and type 2 DM in the dental office.21Marino R, et al. Attitudes and opinions of oral healthcare professionals on screening for Type-2 diabetes. BMC Health Serv Res. 2021;21(1):743 https://www.ncbi.nlm.nih.gov/pubmed/34315460. Using a questionnaire that allowed for explanation of responses, the oral health care providers were supportive of the idea of screening for pre-DM and type 2 DM but identified for potential barriers to implementation of such a program.
- Oral health care providers have limited knowledge about how to screen for dysglycemia.
- Patients may not be aware of the connection between DM and oral disease, and therefore may not be comfortable with oral health care providers offering this service.
- There is a financial concern about payment/reimbursement for the screening procedure.
- There are scope of practice and medical-legal concerns associated with screening for dysglycemia in the dental office.
In addition, the need for communication and collaboration between oral health care providers and medical providers is essential. A positive finding (patients whose POC test result is in the pre-DM or DM range) only benefits the patient if there is medical follow-up to determine the diagnosis (these screening tests are not a diagnosis, which only can be made by the person’s medical provider and initiate appropriate treatment), and appropriate treatment.
Of the four points raised in the study,21Marino R, et al. Attitudes and opinions of oral healthcare professionals on screening for Type-2 diabetes. BMC Health Serv Res. 2021;21(1):743 https://www.ncbi.nlm.nih.gov/pubmed/34315460. the first and second can be addressed by educating the oral health care provider, who should both understand these relationships and be comfortable explaining background information to patients. The third and fourth points are more complicated. At present, dental insurance and medical insurance are unlikely to cover the cost of POC testing for dysglycemia in the dental office, so this may be an out-of-pocket expense for the patient. The matter of whether this activity falls within the scope of dental practice is likely determined by each state, and contact with the state dental association, or the local board of health is suggested. An associated concern is the regulatory issues that govern the use of screening tests in health care facilities. This is addressed by the Clinical Laboratory Improvement Amendments or CLIA. The screening tests that would be employed in a dental office should be “waived tests”, which means that they have been identified as simple to perform, with a low risk of inaccurate results. More information can be found at www.cdc.gov/clia/index.html.
Patient and medical provider awareness of the association between DM and periodontal disease has also been recently addressed22Siddiqi A, et al. Awareness of diabetic patients regarding the bidirectional association between periodontal disease and diabetes mellitus: A public oral health concern. J Contemp Dent Pract. 2020;21(11):1270-4 https://www.ncbi.nlm.nih.gov/pubmed/33850074. and only one-third of the surveyed patients recall being asked by their medical provider about their oral health. More than half were not aware of the association between DM and periodontal disease. This confirms earlier reports.
Other reports confirm that patients with DM generally do not understand the relationship of DM and both periodontal disease and dental caries.23Parakh MK, et al. Knowledge and awareness of oral manifestations of diabetes mellitus and oral health assessment among diabetes mellitus patients - A cross sectional study. Curr Diabetes Rev. 2020;16(2):156-64 https://www.ncbi.nlm.nih.gov/pubmed/31057116. Based on a 12-item questionnaire about the relationship of DM and oral disease, the average score of a group of 447 patients with DM was only 4.92. Another study asked patients with DM about their knowledge of the DM-oral disease relationship. About 80% had received treatment for periodontitis, but only 30% reported receiving information about the association of DM and periodontitis.24Valentim FB, et al. The importance of integrated healthcare in the association between oral health and awareness of periodontitis and diabetes in type 2 diabetics. Oral Health Prev Dent. 2021;19(1):1-6 https://www.ncbi.nlm.nih.gov/pubmed/33491372. These findings agree with previously published information and emphasize the need for improved communication between oral health providers, patients, and other health care professionals.
The Relationship of Preventive Dental Care and General Health Outcomes
The final topic to be reviewed is controversial yet represents a potentially ground-breaking aspect of the systemic disease-oral disease relationship. For DM, this refers to findings suggesting that provision of preventive dental care/conservative periodontal treatment is associated with improved health care outcomes (reduced utilization and lower costs). The development of this research theme is the outcome of earlier studies and represents a logical extension of this entire area of investigation.
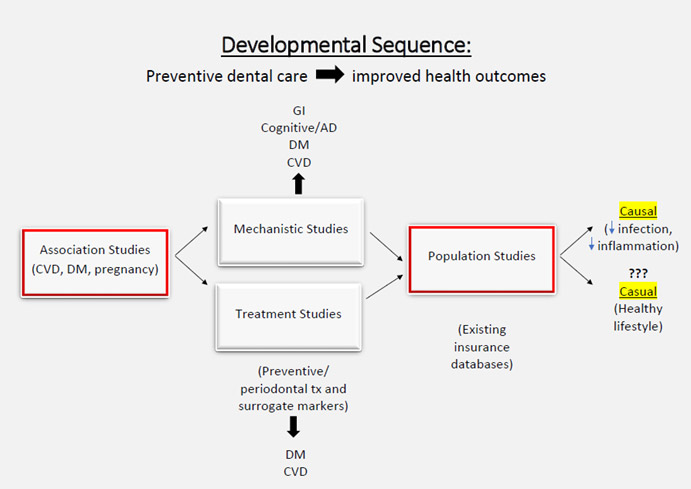
Tracing the development of a discipline referred to as “Periodontal Medicine”, the first studies identified cross-sectional associations between periodontal disease and several chronic diseases, most notably cardiovascular/cerebrovascular disease and diabetes mellitus, as well as adverse pregnancy outcomes. These reports, which were confirmed by investigators across the U.S. as well as globally, were followed by two lines of investigation:1) treatment studies to determine if conservative treatment could improve health outcomes, and 2) mechanistic studies, generally using animal models, to define mechanisms to explain how oral infection/oral inflammation could contribute to certain chronic diseases (see Figure 2).
The clinical treatment studies utilized surrogate markers for chronic disease, most notably HbA1c for DM. While a clinical trial that had a clinical endpoint (i.e., retinopathy or nephropathy for DM) would be ideal such studies that would require a time course measured in years, and many hundreds of patients, with a prohibitive cost. The mechanistic studies sought to demonstrate biological plausibility by using animal models to demonstrate how the chronic disease was adversely affected by periodontal infection and inflammation.
With this information as background, investigators have examined existing databases to assess the relationship between preventive dental care/conservative periodontal therapy and health outcomes. These outcomes include utilization of the emergency department and the number of hospitalizations, as well as associated costs. The first study was published in 2014.25Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519. Using insurance claims data, the relationships were examined for insured individuals with DM, coronary artery disease, cerebrovascular disease, rheumatoid arthritis, and pregnancy. They reported that medical costs were significantly reduced for persons in 4 of the 5 chronic disease categories (all except rheumatoid arthritis) who received complete periodontal treatment. The reductions were 40.2%, 40.9%, 10.7% and 73.7%, respectively. Similar reductions were seen for hospitalizations. However, these findings have been challenged,26Sheiham A. Claims that periodontal treatment reduces costs of treating five systemic conditions are questionable. J Evid Based Dent Pract. 2015;15(1):35-6 https://www.ncbi.nlm.nih.gov/pubmed/25666581. based on a lack of clarity about the control group and a very small number of patients who met the criteria for having received complete periodontal treatment (out of a population of more than 338,000 enrollees, 1% or less met the criteria). Further, there were concerns about adequate consideration of confounding variables, for example characteristics such as living a healthy lifestyle, avoidance of smoking, and weight control. These confounding variables, which were not available in the database, could be an explanation for the findings.
Another U.S. commercial insurance database was used to explore this relationship specifically for persons with DM.27Nasseh K, et al. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-27 https://www.ncbi.nlm.nih.gov/pubmed/26799518. For newly diagnosed persons, a “periodontal intervention” was associated with a reduction in health care costs of $1799 and lower DM-related health care costs of $408. A more recent study from the Netherlands found similar results.28Smits KPJ, et al. Effect of periodontal treatment on diabetes-related healthcare costs: A retrospective study. BMJ Open Diabetes Res Care. 2020;8(1) https://www.ncbi.nlm.nih.gov/pubmed/33099508. Using a Dutch health insurance database, lower DM-related health care costs were observed for those individuals with periodontitis who in the previous year received periodontal therapy. Yet another study from Germany29Blaschke K, et al. The impact of periodontal treatment on healthcare costs in newly diagnosed diabetes patients: Evidence from a German claims database. Diabetes Res Clin Pract. 2021;172:108641 https://www.ncbi.nlm.nih.gov/pubmed/33359573. also used insurance data, and persons with DM who received periodontal therapy had lower total health care costs (4%), hospital costs (13%) and DM-related pharmacy costs (7%).
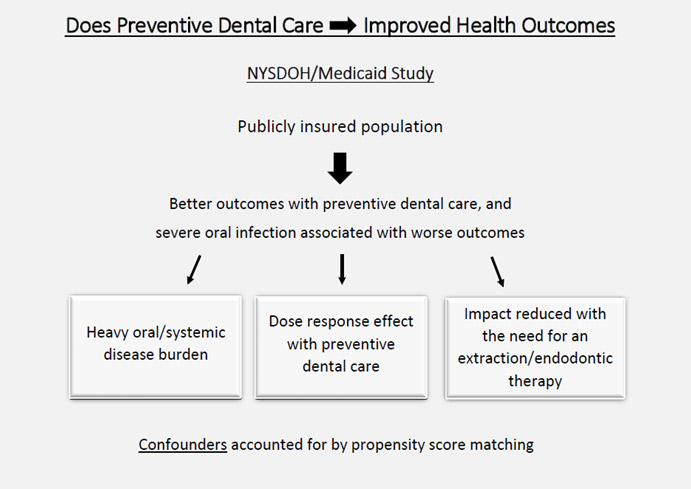
To answer some of the open questions, a recent report examined a publicly insured population from New York State, evaluating the relationship of preventive dental care to health outcomes, including emergency department visits and hospitalizations, as well as costs associated with utilization of these services, plus both pharmacy and total health care costs.30Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960. Here the comparison was between enrollees in the NYS Medicaid program who did, and did not, access dental services. This database was important to study because the NYS Medicaid program provides the most robust adult dental benefits of any state. A total of 518,689 members, ages 42 to 64 years of age at the conclusion of the study, who were continuously enrolled for 3 years, were evaluated. Dental services in years 1 and 2 were compared to health outcomes in year 3. Consideration of potentially confounding factors included adjustment for 15 variables (examples include a well-person medical visit and categorized health status). Accounting for these confounding variables will strengthen the association of the two variables of interest, that is utilization of dental services and health outcomes (Figure 3).
Following adjustment for the available confounding variables, members who received at least one preventive dental care (PDC) visit, but did not require an extraction or endodontic therapy, had significantly lower health care utilization and lower health care costs than those in the population who did not access any dental services. Of importance, there was also an adverse effect of requiring an extraction and/or endodontic therapy. These associations were most notable for hospital/inpatient utilization and costs. As examples, those who received a PDC visit without the need for an extraction and/or endodontic therapy had $380 less inpatient cost compared to those who did not have any dental care. If a person had a PDC visit and required an extraction and/or endodontic therapy this reduction was $304. In contrast, if a person had an extraction and/or endodontic therapy without a PDC, there was no difference compared to members who did not receive any dental care. Further, the negative effect of requiring an extraction and/or endodontic therapy in the absence of a PDC visit was seen clearly for total health care costs. These annual costs were $530 greater than those who did not have any dental care. Lastly, a “dose response” effect was observed. The Medicaid program allows two PDC visits per year, for a maximum of 4 over the two-year period. The effect of adding one PDC visit was a 3% reduction in ED use and a 9% reduction in hospital admissions. The addition of each PDC visit was also associated with a $181 decrease in inpatient costs.
A subsequent evaluation of persons in the Medicaid program with chronic diseases (cardiovascular disease, diabetes mellitus, respiratory disease, and cognitive impairment) who received a PDC visit revealed greater reductions in health care utilization and costs compared to enrollees who did not access dental services. These data indicate that reduced utilization and costs associated with PDC in the NYS Medicaid program were being driven primarily by enrollees with chronic diseases.
These studies indicate an association of preventive dental care with improved health outcomes, most notably reduced hospital visits and lower inpatient costs. The challenge here is to determine cause and effect, which is difficult to establish since these studies utilize existing insurance databases to examine these relationships. These databases were not designed to specifically answer the questions being asked. To narrow down the possibility that some other variable is dramatically influencing the association, consideration of confounding variables must be part of the analysis. Given the potential significance of the finding that preventive dental care can reduce the need for health care services and lower health care costs, this question will undoubtedly continue to be studied.
Concluding remarks
This essay emphasizes the continued expansion of our understanding of the relationship between oral disease and systemic disease, best illustrated for persons with DM. In addition to the impact of dysglycemia on the oral cavity discussed in the first two essays in this series and the first part of this essay, the last two topics covered here clearly emphasize the need for the dental profession to consider its relationship with the larger health care system. Evidence that persons with previously detected pre-DM and DM can be identified in dental clinical settings, and that preventive dental care is associated with improved health outcomes, lead to the conclusion that close alignment of dental and medical care will improve both oral health and general health of our patients, primarily older adults. It is incumbent on both dental and medical professions to work towards this goal.
Legends for Figures:
Figure 1
Figure 1A: Acute atrophic candidiasis, as evidenced on the dorsal of the tongue.
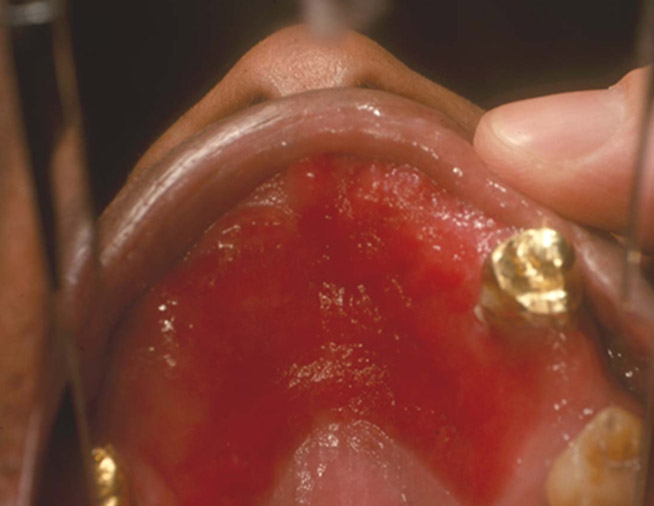
Figure 1B: Chronic atrophic candidiasis, which is obvious under a partial denture in the maxilla.
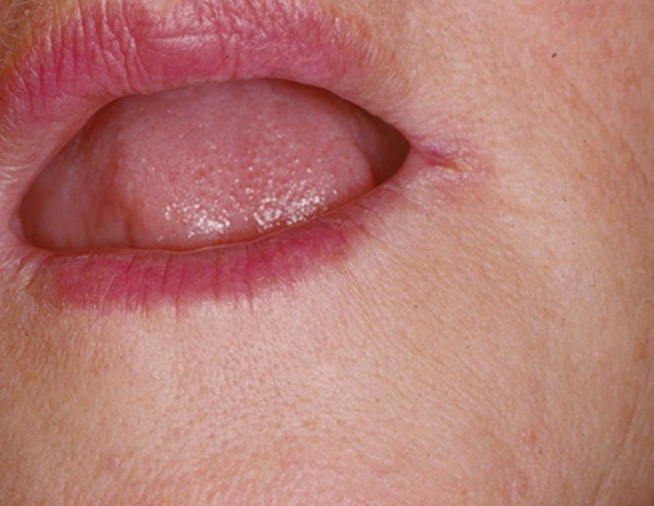
Figure 1C: Angular cheilitis, which is often overlooked as a manifestation of Candida infection.
Figure 2: Earlier research has led to an examination of the relationship of preventive dental care to health outcomes. These studies rely on the analysis of existing insurance databases which contain both medical and dental data.
Figure 3: The study of the relationship between dental care and health outcomes utilizing the New York State Medicaid database (Lamster et. al., 2021).
- Figure 1A: Acute atrophic candidiasis
- Figure 1B: Chronic atrophic candidiasis (“denture stomatitis”)
- Figure 1C: Angular Cheilitis
- Figure 2
- Figure 2
References
- 1.Ramos-Garcia P, et al. Diabetes mellitus and oral cancer/oral potentially malignant disorders: A systematic review and meta-analysis. Oral Dis. 2021;27(3):404-21 https://www.ncbi.nlm.nih.gov/pubmed/31994293.
- 2.Mekala MR, et al. Association of diabetes with oral cancer - an enigmatic correlation. Asian Pac J Cancer Prev. 2020;21(3):809-14 https://www.ncbi.nlm.nih.gov/pubmed/32212811.
- 3.Bookout GP, et al. Burning Mouth Syndrome. StatPearls. Treasure Island (FL)2021.
- 4.Patel PN, et al. Oral candidal speciation, virulence and antifungal susceptibility in type 2 diabetes mellitus. Diabetes Res Clin Pract. 2017;125:10-9 https://www.ncbi.nlm.nih.gov/pubmed/28131069.
- 5.Bhuyan L, et al. Candida species diversity in oral cavity of type 2 diabetic patients and their In vitro antifungal susceptibility. Contemp Clin Dent. 2018;9(Suppl 1):S83-S8 https://www.ncbi.nlm.nih.gov/pubmed/29962770.
- 6.Nouraei H, et al. Potential pathogenicity of candida species isolated from oral cavity of patients with diabetes mellitus. Biomed Res Int. 2021;2021:9982744 https://www.ncbi.nlm.nih.gov/pubmed/34136578.
- 7.Javed F, et al. Oral Candida carriage and species prevalence in denture stomatitis patients with and without diabetes. J Biol Regul Homeost Agents. 2017;31(2):343-6 https://www.ncbi.nlm.nih.gov/pubmed/28685534.
- 8.Yeter HH, et al. Oral candida colonization as a risk factor for chronic inflammation and atherosclerosis in hemodialysis patients. Ther Apher Dial. 2019;23(6):542-9 https://www.ncbi.nlm.nih.gov/pubmed/30895718.
- 9.Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services; 2020.
- 10.Chasens ER, et al. Citizenship and health insurance status predict glycemic management: NHANES data 2007-2016. Prev Med. 2020;139:106180 https://www.ncbi.nlm.nih.gov/pubmed/32593731.
- 11.Thorpe LE, et al. Change in diabetes prevalence and control among New York City adults: NYC Health and Nutrition Examination Surveys 2004-2014. J Urban Health. 2018;95(6):826-31 https://www.ncbi.nlm.nih.gov/pubmed/29987771.
- 12.Glurich I, et al. Screening for dysglycaemia in dental primary care practice settings: Systematic review of the evidence. Int Dent J. 2018;68(6):369-77 https://www.ncbi.nlm.nih.gov/pubmed/29740815.
- 13.Chinnasamy A, Moodie M. Prevalence of Undiagnosed Diabetes and Prediabetes in the Dental Setting: A Systematic Review and Meta-Analysis. Int J Dent. 2020;2020:2964020 https://www.ncbi.nlm.nih.gov/pubmed/32908510.
- 14.Yonel Z, et al. Use of dental practices for the identification of adults with undiagnosed type 2 diabetes mellitus or non-diabetic hyperglycaemia: A systematic review. Diabet Med. 2020;37(9):1443-53 https://www.ncbi.nlm.nih.gov/pubmed/32426909.
- 15.Estrich CG, et al. Prediabetes and diabetes screening in dental care settings: NHANES 2013 to 2016. JDR Clin Trans Res. 2019;4(1):76-85 https://www.ncbi.nlm.nih.gov/pubmed/30596147.
- 16.Su N, et al. Development and validation of a screening model for diabetes mellitus in patients with periodontitis in dental settings. Clin Oral Investig. 2020;24(11):4089-100 https://www.ncbi.nlm.nih.gov/pubmed/32542584.
- 17.Philips KH, et al. Periodontal disease, undiagnosed diabetes, and body mass index: Implications for diabetes screening by dentists. J Am Dent Assoc. 2021;152(1):25-35 https://www.ncbi.nlm.nih.gov/pubmed/33256949.
- 18.Grigoriadis A, et al. Prediabetes/diabetes screening strategy at the periodontal clinic. Clin Exp Dent Res. 2021;7(1):85-92 https://www.ncbi.nlm.nih.gov/pubmed/33300692.
- 19.Montero E, et al. Screening of undiagnosed hyperglycaemia in the dental setting: The DiabetRisk study. A field trial. J Clin Periodontol. 2021;48(3):378-88 https://www.ncbi.nlm.nih.gov/pubmed/33263197.
- 20.Goh G, et al. The prevalence of potentially undiagnosed type II diabetes in patients with chronic periodontitis attending a general dental practice in London - a feasibility study. Br Dent J. 2021;231(3):180-6 https://www.ncbi.nlm.nih.gov/pubmed/34385649.
- 21.Marino R, et al. Attitudes and opinions of oral healthcare professionals on screening for Type-2 diabetes. BMC Health Serv Res. 2021;21(1):743 https://www.ncbi.nlm.nih.gov/pubmed/34315460.
- 22.Siddiqi A, et al. Awareness of diabetic patients regarding the bidirectional association between periodontal disease and diabetes mellitus: A public oral health concern. J Contemp Dent Pract. 2020;21(11):1270-4 https://www.ncbi.nlm.nih.gov/pubmed/33850074.
- 23.Parakh MK, et al. Knowledge and awareness of oral manifestations of diabetes mellitus and oral health assessment among diabetes mellitus patients - A cross sectional study. Curr Diabetes Rev. 2020;16(2):156-64 https://www.ncbi.nlm.nih.gov/pubmed/31057116.
- 24.Valentim FB, et al. The importance of integrated healthcare in the association between oral health and awareness of periodontitis and diabetes in type 2 diabetics. Oral Health Prev Dent. 2021;19(1):1-6 https://www.ncbi.nlm.nih.gov/pubmed/33491372.
- 25.Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519.
- 26.Sheiham A. Claims that periodontal treatment reduces costs of treating five systemic conditions are questionable. J Evid Based Dent Pract. 2015;15(1):35-6 https://www.ncbi.nlm.nih.gov/pubmed/25666581.
- 27.Nasseh K, et al. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-27 https://www.ncbi.nlm.nih.gov/pubmed/26799518.
- 28.Smits KPJ, et al. Effect of periodontal treatment on diabetes-related healthcare costs: A retrospective study. BMJ Open Diabetes Res Care. 2020;8(1) https://www.ncbi.nlm.nih.gov/pubmed/33099508.
- 29.Blaschke K, et al. The impact of periodontal treatment on healthcare costs in newly diagnosed diabetes patients: Evidence from a German claims database. Diabetes Res Clin Pract. 2021;172:108641 https://www.ncbi.nlm.nih.gov/pubmed/33359573.
- 30.Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960.