Does preventive dental care/conservative periodontal treatment improve health outcomes for patients with chronic diseases?
“Periodontal Medicine” is the discipline that studies the relationship of periodontal disease to systemic disease, with a focus on periodontitis as a risk factor for chronic diseases. These studies have expanded to include other oral infections such as endodontic disease. The underlying premise is that oral infection, and the resultant inflammatory response, can adversely affect chronic diseases. Published research on this topic includes epidemiologic surveys, clinical trials, animal models and cell function studies. From the clinical perspective, it is important to define the effect of periodontal therapy on chronic disease to determine if preventive dental care/conservative periodontal treatment can improve health outcomes.
The introduction of “Periodontal Medicine” can be traced to a conference held in 1997 in Chapel Hill, North Carolina. The proceedings of that conference were published in 19981Stamm JW. Periodontal diseases and human health: new directions in periodontal medicine. Ann Periodontol. 1998;3(1):1-2 https://www.ncbi.nlm.nih.gov/pubmed/9722684.. In the 25 years since that meeting, this area of study has developed into one of the most important in dentistry.
The focus of these studies is on non-communicable, chronic diseases (NCDs), of which cardiovascular disease (CVD), diabetes mellitus (DM), respiratory diseases and pregnancy outcomes (included here but not a chronic condition or disease) have been the most intensely studied. However, associations have been reported for more than 50 other diseases and disorders.
Background and supporting evidence
Research on this topic has been published in traditional medical, dental, and public health journals, alerting both dental and non-dental health professionals to the general importance of oral health as part of general health. This body of work has contributed to the discussion about medical-dental integration and serves to remind our health care colleagues that the oral cavity is, of course, a part of the body, and should not be considered separately, as the biological principles are the same in the oral cavity as elsewhere in the body.
As this discipline advanced, clinical studies examined how surrogate markers of chronic diseases were affected by preventive dental care/conservative periodontal treatment. The prime example is the effect on glycated hemoglobin (HbA1c) in blood as an indicator of metabolic control in DM. This marker provides a measure of the concentration of glucose in blood over a 2-to-3-month period, reflective of the combination of hemoglobin and glucose, a reaction that is determined solely on the concentration of glucose in the blood. As red blood cells have a half-life of 2-3 months, measurement of HbA1c reflects the level of metabolic control over this period. Studies have shown that elevated levels of HbA1c in blood are associated with increased risk of developing clinical complications of DM, including retinopathy2Zhang B, et al. The value of glycosylated hemoglobin in the diagnosis of diabetic retinopathy: a systematic review and Meta-analysis. BMC Endocr Disord. 2021;21(1):82 https://www.ncbi.nlm.nih.gov/pubmed/33902557. and nephropathy3Lin CH, et al. Hemoglobin glycation index predicts renal function deterioration in patients with type 2 diabetes and a low risk of chronic kidney disease. Diabetes Res Clin Pract. 2022;186:109834 https://www.ncbi.nlm.nih.gov/pubmed/35314255..
Many studies have examined the effect of preventive dental care/conservative periodontal treatment on levels of HbA1c in persons with DM. A recent Cochrane Library review examined “Treatment of periodontitis for glycemic control in people with diabetes mellitus”4Simpson TC, et al. Treatment of periodontitis for glycaemic control in people with diabetes mellitus. Cochrane Database Syst Rev. 2022;4:CD004714 https://www.ncbi.nlm.nih.gov/pubmed/35420698.. This systemic review included 35 studies and a total of 3,245 patients. The focus was on persons with type 2 diabetes, and follow-up ranged from 3 to 12 months. This review considered the risk of bias present in each study.
The major conclusion was that at 3 months after treatment the reduction in HbA1c was 0.43%, 0.30% at 6 months and 0.50% at 12 months. The authors stated that the results reported has necessitated “a change in our conclusions about the primary outcome of glycaemic control in our level of certainty in this conclusion. We now have evidence that periodontal treatment using subgingival instrumentation improves glycaemic control in people with both periodontitis and diabetes by a clinically significant amount when compared to no treatment or usual care”. This is a change from the previous Cochrane review, which concluded that there was insufficient evidence to state that periodontal therapy had this beneficial effect. Further, strengthening the conclusion, the review stated that additional studies are not likely to change the outcome.
Another example of a surrogate marker of chronic disease is vascular function, measured as bronchial artery stiffness, which has been identified as a risk factor for CVD. This indicator of risk for developing cardiovascular disease was evaluated in relation to periodontal treatment5Tonetti MS, et al. Treatment of periodontitis and endothelial function. N Engl J Med. 2007;356(9):911-20 https://www.ncbi.nlm.nih.gov/pubmed/17329698., and was associated with reduced arterial stiffness.
Analysis of ‘Big Data’ sets
After determining that preventive dental care/conservative periodontal treatment could reduce surrogate markers of different chronic diseases, the next logical next step was to evaluate the effect of this treatment on development of clinical complications of these chronic diseases. For DM, this would mean development of clinical complication, which include retinopathy and nephropathy, and for CVD this could be the onset of angina, occurrence of a myocardial infarction, or a second myocardial infarction in persons at increased risk for such a second event. However, such studies require a lengthy prospective design, large numbers of patients, and appropriate controls that consider all aspects of care for persons with DM or CVD (i.e., initial level of disease severity, medications, and other interventions, with balancing of test and control groups). The cost of such studies would be prohibitive, and consequently have not been performed.
Another approach was sought to examine the clinical effects of preventive dental care/conservative periodontal treatment on health outcomes. This led to the analyses of large insurance databases that contain medical and dental treatment and health outcomes data. These databases have been analyzed to determine if there is an association between provision of preventive dental care/conservative periodontal treatment and health outcomes (both utilization and cost) in persons with NCDs.
The first of the studies to examine the relationship between provision of conservative periodontal treatment and specific health outcomes was published in 20146Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519.. A combined database from United Concordia (dental insurance claims) and Highmark, Inc. (medical insurance claims) was analyzed. There was a total of 338,891 individuals where both dental and medical claims data were available. Patients with a medical diagnosis of type 2 DM, coronary artery disease, cerebral vascular disease, rheumatoid arthritis and pregnancy were studied. The outcomes evaluated were total medical costs and number of hospitalizations. The comparisons were between those individuals who were and were not treated for periodontal disease.
Their analysis revealed significant reductions in both costs and hospitalizations for those receiving periodontal treatment versus no treatment for DM, coronary artery disease, cerebrovascular disease, and pregnancy, but not rheumatoid arthritis. The authors concluded that these findings agreed with the earlier evidence that treatment of “active periodontal disease” has a systemic effect that goes beyond improving the status of the periodontium. They also advocated for inclusion of such treatment in the management of chronic diseases.
This study attracted considerable attention, and was criticized in a commentary7Sheiham A. Claims that periodontal treatment reduces costs of treating five systemic conditions are questionable. J Evid Based Dent Pract. 2015;15(1):35-6 https://www.ncbi.nlm.nih.gov/pubmed/25666581.. Several critical shortcomings where identified, which included:
- The criteria for periodontal care was 4 visits of treatment. If 1, 2 or 3 visits were received than that individual was considered as a control (untreated). Considering the large number of persons in the database, only 913 DM patients received treatment (control group numbered 90,329), 139 coronary artery disease patients were treated (12,868 controls), 90 cerebrovascular disease patients (8,368 controls), 27 pregnant women (10,851 controls) and 536 rheumatoid arthritis patients (80,903 controls). This imbalance was considered a significand design flaw.
- Given the criteria for assignment to the test group, some individuals in the control group also received periodontal treatment. This raises the concern if they were a true control group.
- The lack of data concerning the severity of periodontal disease at the outset of the period of observation is a major omission.
- The treated group may have been composed of individuals who complied with all treatment suggestions and were therefore inherently different than the controls.
Jeffcoat replied to this critique8Jeffcoat M. Periodontal Therapy and Systemic Disease: An Author's View. J Evid Based Dent Pract. 2015;15(3):140-2 https://www.ncbi.nlm.nih.gov/pubmed/26337590.. She argued that answering the question “Does periodontal therapy have an impact on health costs” can only be accomplished with analysis of large databases since a full-scale randomized control trial is a desirable but impractical approach. Also acknowledged were shortcomings associated with using large databases, including the absence of important variables such as the medical history, weight (or body mass index/BMI) and history of smoking. However, a distinct advantage of using an available database is the large number of records (here 338,891 individuals), resulting in great statistical power.
The publication of the Jeffcoat et al study6Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519. and the Sheiham critique7Sheiham A. Claims that periodontal treatment reduces costs of treating five systemic conditions are questionable. J Evid Based Dent Pract. 2015;15(1):35-6 https://www.ncbi.nlm.nih.gov/pubmed/25666581. noting concerns about the study design and methodology heightened interest in the use of large data sets to determine if there was an association between preventive dental care/conservative periodontal treatment and improved health outcomes. A number of related studies have subsequently been published.
A report from the American Dental Association’s Health Policy Institute used the Truven Market Scan ® Research Databases, which contained medical, dental and pharmacy claims data. The relationship of periodontal treatment to health care costs and utilization for persons with recently diagnosed type 2 DM was examined9Nasseh K, et al. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-27 https://www.ncbi.nlm.nih.gov/pubmed/26799518..
A comparison was made between individuals with DM who received periodontal treatment within a two-year period after their DM diagnosis, and those that did not receive such care. Total health care costs (including medications), the sum of total inpatient and outpatient medical costs and total costs related to diabetes care in the 3rd and 4th years after the diagnosis of DM were evaluated. There were 15,002 individuals in the database, with an age range of 18 to 64 years.
For those individuals who had a periodontal intervention, total net health care cost savings were $1,328 over 2 years (years 3 and 4). Total type 2 DM-related costs savings were $408. However, these savings were only seen for those individuals also did not begin drug treatment for DM.
These investigators acknowledged that certain information such as levels of HbA1c was not available in their database. They did, however, consider other potential confounders that were available, including age, gender, and medical status.
Subsequently, a study from the Netherlands examined an insurance database of claims for enrollees with diabetes who did and did not have periodontal treatment10Smits KPJ, et al. Effect of periodontal treatment on diabetes-related healthcare costs: A retrospective study. BMJ Open Diabetes Res Care. 2020;8(1) https://www.ncbi.nlm.nih.gov/pubmed/33099508.. All individuals were continuously enrolled between 2012 and 2018. Identification of cases and controls was based on having at least one DM-related claim in 2012. A comparison was made between enrollees with DM who had or did not have periodontal treatment (total cohort was 41,598 enrollees, 8,188 who received periodontal treatment, and 33,409 who did not). Over the course of the next 6 years, the mean quarterly DM-related health care costs were €38.45, which considered diagnostic assessments, any treatment, required medications, and hospital-related costs. However, for those enrollees who had periodontal treatment, a reduction of €12.03 per quarter in diabetes-related health care costs was seen. While the costs per quarter were small, the percentage reduction in costs associated with provision of conservative periodontal therapy was 31%.
The authors emphasized that all health care providers should be aware of the periodontal status of persons with DM, and the need for treatment if periodontitis is present. They suggested that an association between periodontal treatment and reduced health care costs for persons with DM argues for better coordination of care between physicians and dentists when treating such patients.
In 2021, Lamster et al11Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960. reported on the relationship of preventive dental care (including conservative periodontal care) to health outcomes in the New York State (NYS) Medicaid program. Examining this database offered some unique advantages:
- Medicaid programs provide health insurance for a publicly insured population with a heavy chronic disease and oral disease burden.
- In addition to medical benefits, the NYS Medicaid program provides a relatively robust range of adult dental benefits. Therefore, the database contains data about medical diagnoses and treatment, as well as dental treatment.
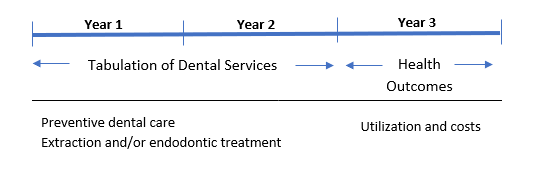
All eligible enrollees between the ages of 40 and 62 years of age at the initiation of the trial, who were continuously enrolled for 3 years, were included. A total of 518,689 records were available for analysis. Older adults (65 years of age and older) were not included because medical care for these individuals is provided through the Medicare program, and that data was not in the NYS Medicaid database. Dental services received in the first two years of the study were evaluated in reference to health outcomes (costs and utilization of services) in the third year (Figure 1). The analyses focused on the relationship of preventive dental care (PDC) to visits to a hospital emergency department (ED) and hospital inpatient admissions (IP), and costs of the emergency department visits, inpatient admissions, pharmacy costs and total adjusted health care costs. Also considered was the need for an extraction or endodontic therapy as surrogate indicators of advanced dental infection. Propensity scores were calculated to adjust for potentially confounding variables. Propensity score analysis is specifically designed to assess the effect of treatment or intervention on an outcome using observational data.
Rates of admission to the ED were lower for members with at least one PDC visit without an extraction or endodontic treatment as compared to those who did not receive dental care (Table 1). IP rates were lower for members who received a PDC without an extraction/endodontic therapy (14%), as well as a PDC and an extraction/endodontic therapy (11%) compared to enrollees who did not receive dental care.
As for costs, differences in the cost of ED differed little among the groups. However, for IP costs, receiving a PDC visit was associated with lower costs as compared to enrollees who did not receive dental care (ranging from -$379 for PDC without an extraction/endodontic therapy to -$304 for PDC and an extraction/endodontic therapy). No reduction was seen if enrollees received an extraction/endodontic therapy but not PDC. There were only minor differences in pharmacy costs among the groups. As for total health care costs, enrollees requiring an extraction or endodontic treatment had higher total health care costs as compared to enrollees who did not receive dental care (Table 1).
Of particular importance, an incremented, beneficial effect of additional PDC visits on outcomes was observed. The Medicaid program allows 2 PDC visits per year, which would be up to 4 visits in the two-year observational period. Each additional PDC visit was associated with a 3% decrease in the relative risk for an ED visit, and a 9% reduction in the risk for an IP admission. Further, health care costs were reduced with each additional PDC visit. This was most pronounced for total adjusted health care costs.
A subsequent analysis of the NYS Medicaid program database evaluated enrollees with DM, comparing those members with diabetes who did and did not receive dental care. Receiving a PDC visit was associated with lower rates of healthcare utilization and costs12Lamster IB, et al. Preventive dental care is associated with improved health care outcomes and reduced costs for Medicaid members with diabetes. Front Dent Med 3:952182. 2022.. Enrollees with DM who received a PDC, but did not require an extraction or endodontic treatment, had a lower rate of ED use. In contrast, those enrollees who had an extraction or endodontic treatment had a higher rate of ED use. Having a PDC was also associated with a reduction in IP admissions. The most notable association was a reduction in IP costs with receiving a PDC visit. This was not seen for enrollees who received an extraction or endodontic treatment. The reduction ranged up to -$823.02 for enrollees with a PDC but without an extraction or endodontic treatment. In addition, lower total adjusted health care costs were seen for enrollees with a PDC, ranging from -$538.84 to -$983.88. Again, requiring an extraction or endodontic treatment was not associated with a reduction in costs (Table 2).
In addition, as seen for the entire cohort, an incremental effect of additional PDC visits on utilization and costs were seen. For each additional PDC visit, ED costs were reduced 4% and IP admissions by 11%. This incremental effect was also seen for health care costs, as each additional PDC visit was associated with an average reduction in IP costs (-$407.58), and total adjusted health care costs (-$665.74).
These two studies were particularly noteworthy for the following reasons:
- This was the first report of the association of preventive dental care and general health outcomes in a publicly insured population with heavy oral and systemic disease burdens.
- The improved outcomes were most pronounced for hospitalizations. Hospital costs account for 70% of the healthcare costs for persons with a chronic disease13Joo JY, Liu MF. Case management effectiveness in reducing hospital use: a systematic review. Int Nurs Rev. 2017;64(2):296-308 https://www.ncbi.nlm.nih.gov/pubmed/27861853..
- These studies demonstrated an incremental, positive effect of additional preventive care visits on health outcomes (utilization and costs).
- The need for an extraction or endodontic treatment, both surrogate indicators of advanced dental infection, reduced the association of preventive care and lower utilization and costs.
- The lower utilization and costs associated with preventive dental care were more pronounced for the enrollees with chronic disease (here DM), as compared to the entire cohort.
- In an effort to reduce the influence of confounding variable, these two studies adjusted the analyses for 15 variables in the database, including the severity of systemic disease and receiving a well-person medical visit.
However, it is important to note that other potential confounding variables such as weight/body mass index and smoking were not available in the database.
Another study that examined the association of preventive dental care and health outcomes analyzed data from a commercial healthcare plan in Arkansas14Borah BJ, et al. Association Between Preventive Dental Care and Healthcare Cost for Enrollees With Diabetes or Coronary Artery Disease: 5-Year Experience. Compend Contin Educ Dent. 2022;43(3):130-9 https://www.ncbi.nlm.nih.gov/pubmed/35272460.. The total number of records available for analysis was 19,095, and the outcome measure was the total amount paid by the plan (referred to as “all-cause costs”). Those enrollees who adhered to a plan of preventive dental care (defined as at least one preventive dental care visit in each of the 4 years of the observation period) had reduced costs. This ranged from -$515 to -$574 for enrollees with DM and -$866 to -$1718 for enrollees with DM and CAD. The authors suggested that health plans should include preventive dental care services in their plan, and provide incentives for enrollees to utilize these benefits “to improve health and lower costs for enrollees with diabetes and coronary artery disease.”
Another analysis estimated the annual savings in the United States that may be realized with provision of periodontal treatment for persons with DM or CVD in the Medicare program15Heaton LJ, et al. Another billion reasons for a Medicare dental benefit. Boston, MA: CareQuest Institute, September 2022. DOI: 10.35565/CQI.2022.2006.. Enrollment and cost expenditure data were obtained from the Medicare Current Beneficiary Survey, which is conducted by the Centers for Medicare & Medicaid Services. The estimated per-person savings associated with periodontal treatment for individuals with DM and CVD was based on an analysis conducted by the healthcare insurance company Cigna. The calculation included consideration of Medicare enrollees who were and were not in Medicare Advantage plans, as well as different levels of utilization. In sum, the analysis indicated an estimated annual savings of between $3.6 and $14.5 billion for enrollees with DM, and between $6.9 and $ 27.8 billion for enrollees with CVD.
Reviews examining the findings
Several reviews have been published examining the question “does providing dental services reduce overall health care costs?” Elani et al16Elani HW, et al. Does providing dental services reduce overall health care costs?: A systematic review of the literature. J Am Dent Assoc. 2018;149(8):696-703 e2 https://www.ncbi.nlm.nih.gov/pubmed/29866364. included 3 studies, among which are the reports by Jeffcoat et al.6Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519. and Nasseh et al.9Nasseh K, et al. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-27 https://www.ncbi.nlm.nih.gov/pubmed/26799518., and stated that while 2 studies demonstrated cost reductions, these were too few published papers to draw a conclusion. A review by Taylor et al17Taylor HL, et al. Does Nonsurgical Periodontal Treatment Improve Systemic Health? J Dent Res. 2021;100(3):253-60 https://www.ncbi.nlm.nih.gov/pubmed/33089733. asked the same question and included both systematic reviews and original research. Here a wider range of studies were included, that reported different outcomes (biomarkers, surrogate endpoints such as HbA1c, as well as clinical endpoints). Fifty-two studies were included (21 for DM, 15 for birth outcomes, 8 for CAD, 3 for obesity, 3 for rheumatoid arthritis and 2 for chronic kidney disease). Their conclusions agreed with what was stated by Elani et al16Elani HW, et al. Does providing dental services reduce overall health care costs?: A systematic review of the literature. J Am Dent Assoc. 2018;149(8):696-703 e2 https://www.ncbi.nlm.nih.gov/pubmed/29866364.. Specifically, while the evidence is clear that there is an association of periodontal disease and certain chronic diseases, the evidence is not sufficient to state that preventive dental care/conservative periodontal treatment improves health outcomes in person with certain chronic diseases.
Interpretation of the findings
These studies demonstrate an association between preventive dental care/conservative periodontal treatment and improved general health outcomes with reduced utilization and lower costs. These findings are potentially very impactful. It is important to remember, however, that the databases that are being used to examine these relationships were not designed to answer these questions, so caution is urged in the interpretation of the findings, and what information is conveyed to patients. Nevertheless, given the cost of conducting a case control study that would address the question of cause and effect, the analysis of existing, large databases represents a valid approach to examining these questions.
A commentary that was published in 2022 in the Journal of American Dental Association18Abt E, et al. Periodontal disease and medical maladies: What do we really know? J Am Dent Assoc. 2022;153(1):9-13 https://www.ncbi.nlm.nih.gov/pubmed/34861990. reviewed many of the issues surrounding this area of investigation. These include:
- “Association versus Causality”: because two events are correlated does not imply that one causes the other. They note the importance of other criteria, such as biological plausibility, a dose-response effect and also the relationship of dental treatment to the medical outcome. These criteria were met in the Lamster et al. studies11Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960.,12Lamster IB, et al. Preventive dental care is associated with improved health care outcomes and reduced costs for Medicaid members with diabetes. Front Dent Med 3:952182. 2022. .
- There are drawbacks when using observational, interventional and ‘big data’ studies. As noted, there are concerns when using these types of studies when attempting to demonstrate causality. These include very heterogenous study populations, an underlying risk factor for the purported cause (periodontal disease) and effect (on the chronic disease) such as smoking, use of surrogate markers versus a true disease outcome (reduction in the HbA1c versus reduced occurrence of a clinical complication of DM such as retinopathy), as well as missing variables when analyzing big data sets. They also caution against professional organizations overstating these relationships in their position papers and websites.
- Remember that treating periodontal disease to promote oral health and retention of the dentition is a valuable service. There are many benefits associated with a healthy oral cavity (i.e., proper mastication and the ability to eat a nutritional healthy diet, helping to enhance social interaction and absence of pain). Establishment and maintenance of a heathy mouth is reason alone for providing periodontal treatment when periodontal disease is present.
The critical question is the cause-and-effect relationship of the reported associations.
Is there a CAUSAL effect? The supposition here is that removal of the dental biofilm reduces chronic periodontal inflammation, which reduces the total systemic inflammatory burden, which in turn leads to reduced severity of certain chronic diseases, and lower health care utilization and costs.
Is the relationship CASUAL? The supposition here is that the findings are secondary to the benefits of a healthy lifestyle. The argument is that persons who seek preventive dental care also live a healthy lifestyle, do not smoke, exercise regularly and eat a healthy diet. In this case the effect of preventive dental care cannot be identified as the reason for improved health outcomes, but the findings are indicative of a constellation of patient activities that reduces the impact of chronic diseases19Kushner RF, Sorensen KW. Lifestyle medicine: the future of chronic disease management. Curr Opin Endocrinol Diabetes Obes. 2013;20(5):389-95 https://www.ncbi.nlm.nih.gov/pubmed/23974765.,20Santos L. The impact of nutrition and lifestyle modification on health. Eur J Intern Med. 2022;97:18-25 https://www.ncbi.nlm.nih.gov/pubmed/34670680..
This question cannot be definitively answered. To address the concern, however, these studies must consider what are termed confounding variables. In this case these are lifestyle variables that are factored into the statistical analysis11Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960.,12Lamster IB, et al. Preventive dental care is associated with improved health care outcomes and reduced costs for Medicaid members with diabetes. Front Dent Med 3:952182. 2022..
Conclusions
This review has examined the research findings that have reported an association of preventive dental care/conservative periodontal treatment with improved health outcomes for persons with certain chronic diseases, primarily DM. Also noted are some of the concerns regarding establishing cause and effect for these relationships.
A definitive answer to the fundamental question, that is whether the provision of preventive dental care/conservative periodontal treatment is a means of improving health outcomes for persons with periodontal disease and certain chronic diseases, is not yet available. However, the data that is currently available is intriguing and cannot be ignored. The total number of patient records in the studies reported is more than 900,000, and the later studies make a concerted effort to consider important confounding variables. An affirmative answer, or a consensus in the affirmative, would be a major advance in care for persons with chronic diseases, and substantially alter the relationship of dentistry to general health care, specifically how dental and medical professionals interact in clinical practice.
For now, it is imperative that dental professionals be aware of the latest research in this field and present the facts as they are known to patients and non-dental health care professionals.
References
- 1.Stamm JW. Periodontal diseases and human health: new directions in periodontal medicine. Ann Periodontol. 1998;3(1):1-2 https://www.ncbi.nlm.nih.gov/pubmed/9722684.
- 2.Zhang B, et al. The value of glycosylated hemoglobin in the diagnosis of diabetic retinopathy: a systematic review and Meta-analysis. BMC Endocr Disord. 2021;21(1):82 https://www.ncbi.nlm.nih.gov/pubmed/33902557.
- 3.Lin CH, et al. Hemoglobin glycation index predicts renal function deterioration in patients with type 2 diabetes and a low risk of chronic kidney disease. Diabetes Res Clin Pract. 2022;186:109834 https://www.ncbi.nlm.nih.gov/pubmed/35314255.
- 4.Simpson TC, et al. Treatment of periodontitis for glycaemic control in people with diabetes mellitus. Cochrane Database Syst Rev. 2022;4:CD004714 https://www.ncbi.nlm.nih.gov/pubmed/35420698.
- 5.Tonetti MS, et al. Treatment of periodontitis and endothelial function. N Engl J Med. 2007;356(9):911-20 https://www.ncbi.nlm.nih.gov/pubmed/17329698.
- 6.Jeffcoat MK, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-74 https://www.ncbi.nlm.nih.gov/pubmed/24953519.
- 7.Sheiham A. Claims that periodontal treatment reduces costs of treating five systemic conditions are questionable. J Evid Based Dent Pract. 2015;15(1):35-6 https://www.ncbi.nlm.nih.gov/pubmed/25666581.
- 8.Jeffcoat M. Periodontal Therapy and Systemic Disease: An Author's View. J Evid Based Dent Pract. 2015;15(3):140-2 https://www.ncbi.nlm.nih.gov/pubmed/26337590.
- 9.Nasseh K, et al. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-27 https://www.ncbi.nlm.nih.gov/pubmed/26799518.
- 10.Smits KPJ, et al. Effect of periodontal treatment on diabetes-related healthcare costs: A retrospective study. BMJ Open Diabetes Res Care. 2020;8(1) https://www.ncbi.nlm.nih.gov/pubmed/33099508.
- 11.Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960.
- 12.Lamster IB, et al. Preventive dental care is associated with improved health care outcomes and reduced costs for Medicaid members with diabetes. Front Dent Med 3:952182. 2022.
- 13.Joo JY, Liu MF. Case management effectiveness in reducing hospital use: a systematic review. Int Nurs Rev. 2017;64(2):296-308 https://www.ncbi.nlm.nih.gov/pubmed/27861853.
- 14.Borah BJ, et al. Association Between Preventive Dental Care and Healthcare Cost for Enrollees With Diabetes or Coronary Artery Disease: 5-Year Experience. Compend Contin Educ Dent. 2022;43(3):130-9 https://www.ncbi.nlm.nih.gov/pubmed/35272460.
- 15.Heaton LJ, et al. Another billion reasons for a Medicare dental benefit. Boston, MA: CareQuest Institute, September 2022. DOI: 10.35565/CQI.2022.2006.
- 16.Elani HW, et al. Does providing dental services reduce overall health care costs?: A systematic review of the literature. J Am Dent Assoc. 2018;149(8):696-703 e2 https://www.ncbi.nlm.nih.gov/pubmed/29866364.
- 17.Taylor HL, et al. Does Nonsurgical Periodontal Treatment Improve Systemic Health? J Dent Res. 2021;100(3):253-60 https://www.ncbi.nlm.nih.gov/pubmed/33089733.
- 18.Abt E, et al. Periodontal disease and medical maladies: What do we really know? J Am Dent Assoc. 2022;153(1):9-13 https://www.ncbi.nlm.nih.gov/pubmed/34861990.
- 19.Kushner RF, Sorensen KW. Lifestyle medicine: the future of chronic disease management. Curr Opin Endocrinol Diabetes Obes. 2013;20(5):389-95 https://www.ncbi.nlm.nih.gov/pubmed/23974765.
- 20.Santos L. The impact of nutrition and lifestyle modification on health. Eur J Intern Med. 2022;97:18-25 https://www.ncbi.nlm.nih.gov/pubmed/34670680.
Table 1: Analysis of data from the New York State Medicaid program. change in the average cost per enrollee associated with provision of dental services (entire cohort11Lamster IB, et al. Dental services and health outcomes in the New York State Medicaid Program. J Dent Res. 2021:220345211007448 https://www.ncbi.nlm.nih.gov/pubmed/33880960.).
| Review/Study | Change |
|---|---|
| Any PDC vs. no dental care | -$354.09 (S) |
| PDC without Ext/Endo vs. no dental care | -$379.82 (S) |
| PDC with Ext/Endo vs. no dental care | -$304.64 (S) |
| Ext/Endo (without PDC) vs. no dental care | -$55.63 (NS) |
| Total Health Care | Change |
| Any PDC vs. no dental care | -$81.84 (NS) |
| PDC without Ext/Endo vs. no dental care | -$159.01 (NS) |
| PDC with Ext/Endo vs. no dental care | +$73.40 (NS) |
| Ext/Endo (without PDC) vs. no dental care | +$530.50 (S) |
PDC = preventive dental care.
Ext/Endo = an extraction and/or endodontic treatment.
S = significantly different compared to no dental care group.
NS = not significantly different compared to no dental care group.
Table 2: Analysis of data from the New York State Medicaid program. Change in the average cost per enrollee associated with provision of dental services (enrollees with a diagnosis of diabetes mellitus12Lamster IB, et al. Preventive dental care is associated with improved health care outcomes and reduced costs for Medicaid members with diabetes. Front Dent Med 3:952182. 2022.).
| Inpatient Admissions | Change |
|---|---|
| Any PDC vs. no dental care | -$776.31 (S) |
| PDC without Ext/Endo vs. no dental care | -$823.02 (S) |
| PDC with Ext/Endo vs. no dental care | -$722.62 (S) |
| Ext/Endo (without PDC) vs. no dental care | -$326.91 (NS) |
| Total Health Care | Change |
| Any PDC vs. no dental care | -$881.77 S) |
| PDC without Ext/Endo vs. no dental care | -$983.88 (S) |
| PDC with Ext/Endo vs. no dental care | -$820.37 (S) |
| Ext/Endo (without PDC) vs. no dental care | -$141.37 (NS) |
PDC = preventive dental care.
Ext/Endo = an extraction and/or endodontic treatment.
S = significantly different compared to no dental care group.
NS = not significantly different compared to no dental care group.