Occlusion, Mastication and Cognitive Function
Oral infection (primarily periodontal disease, but also endodontic infection) has been implicated as a risk factor for certain chronic diseases. These relationships are strongest for diabetes mellitus, cardiovascular/cerebrovascular disease, and respiratory disease. Among the other chronic diseases that have been identified as being adversely affected by oral disease is cognitive impairment. Two mechanisms have been proposed to explain this relationship:
1. Influence of infection with a periodontal microorganism.
2. Influence of altered occlusion and limited mastication.
Influence of Infection with a Periodontal Microorganism
Oral infection, and specifically the periodontal pathogen Porphyromonas gingivalis, has been directly implicated in the pathogenesis of dementia (Alzheimer’s disease; AD). A comprehensive report of the role of this periodontal pathogen in AD studied brain tissue collected at autopsy from patients with AD, and also utilized a mouse model. The findings included identification of P. gingivalis in the brains of patients with AD. More specifically, gingipains, which are proteases released by P. gingivalis, were identified in brain tissue from these patients. The level of gingipains correlated with specific brain pathology. Using a mice model, oral infection of mice with P. gingivalis resulted in colonization of the brain, and an increase in amyloid plaques in brain tissue. Further experiments demonstrated that gingipains interfered with nerve function via adverse effects on the tau proteins that are required for normal function. The investigators developed small molecules that inhibited gingipains and found that these inhibitors had a variety of positive effects in their mouse model, including a reduction in P. gingivalis infection in the brain, blockage of amyloid plaque production and a general reduction in neuroinflammation. The authors suggested an important therapeutic application of gingipain inhibitors in AD 1Dominy SS, et al. Porphyromonas gingivalis in Alzheimer's disease brains: Evidence for disease causation and treatment with small-molecule inhibitors. Sci Adv. 2019;5(1):eaau3333 https://www.ncbi.nlm.nih.gov/pubmed/30746447..
Subsequently, several review papers have examined oral infection as a risk factor for cognitive impairment/Alzheimer’s disease. The focus is on P. gingivalis as the offending microorganism.
A review of mechanisms that may be involved has been published2Sadrameli M, et al. Linking mechanisms of periodontitis to Alzheimer's disease. Curr Opin Neurol. 2020;33(2):230-8 https://www.ncbi.nlm.nih.gov/pubmed/32097126.. A variety of oral and airway bacteria, as well as viruses and fungi, have been identified in the brain of patients with AD. Dysbiosis, or imbalance in the microflora would lead to infection in the brain, ultimately resulting in increased production of β-amyloid, which has antimicrobial activity. Given the significance of the accumulation of β-amyloid plagues in the pathogenesis of AD, this would lead to altered brain function and eventual cognitive decline.
A systematic review that examined the link between periodontal disease and AD summarized studies of patients 65 years of age and older 3Borsa L, et al. Analysis the link between periodontal diseases and Alzheimer's disease: A systematic review. Int J Environ Res Public Health. 2021;18(17) https://www.ncbi.nlm.nih.gov/pubmed/34501899.. Five studies were identified. In the oral cavity, there was an increase in several periodontal bacterial species, including P. gingivalis, Fusobacterium nucleatum, Capnocytophaga rectus and Actinomyces naeslundii. If periodontitis was present, over a 6-month period the rate of cognitive decline was 6 times greater for patients with periodontitis as compared to AD patients without periodontitis. The authors suggested that periodontal treatment should be as an approach to prevention of AD.
Another systematic review focused on the importance of P. gingivalis in animal models of AD, and the effect of oral infection with this organism on cognitive function. Nine articles were included. Infection with P. gingivalis, or lipopolysaccharide derived from P. gingivalis, led to a variety of alterations, including an increase in key inflammatory mediators (i.e., tumor necrosis factor α and interleukin-1β), activation of the complement system and increased production of β-amyloid. In terms of changes in the brain, tissue degeneration and cognitive changes were reported. These changes were consistent with AD 4Costa MJF, et al. Relationship of Porphyromonas gingivalis and Alzheimer's disease: A systematic review of pre-clinical studies. Clin Oral Investig. 2021;25(3):797-806 https://www.ncbi.nlm.nih.gov/pubmed/33469718..
Influence of Altered Occlusion and Limited Mastication
The finding that oral infection/periodontal infection appears to be a risk factor for AD is reminiscent of the linkage between oral disease and other chronic diseases. However, the relationship between the development of frank oral disease and cognitive impairment is further supported by other data that examined a different aspect of the oral disease/cognitive function relationship. That is a linkage between occlusion, mastication, and cognitive function. The underlying mechanism to account for increased risk of dementia with poor mastication has not been definitively established but may relate to the reduction in chewing/mastication not stimulating specific areas of the brain. This is a complex interaction and may also relate to the reduced intake of certain nutrients because of poor occlusion and the need to eat a limited diet5Munoz Fernandez SS, Lima Ribeiro SM. Nutrition and Alzheimer disease. Clin Geriatr Med. 2018;34(4):677-97 https://www.ncbi.nlm.nih.gov/pubmed/30336995.,6Aquilani R, et al. Is the Brain Undernourished in Alzheimer's Disease? Nutrients. 2022;14(9) https://www.ncbi.nlm.nih.gov/pubmed/35565839.. Various studies using different approaches offer an explanation for this relationship.
Animal Studies:
Animal studies examining an association between a potential risk factor for a disease (here reduced or impaired mastication) and a disorder (cognitive impairment) provide both biological rationale and a suggestion of the underlying mechanisms that may account for this relationship.
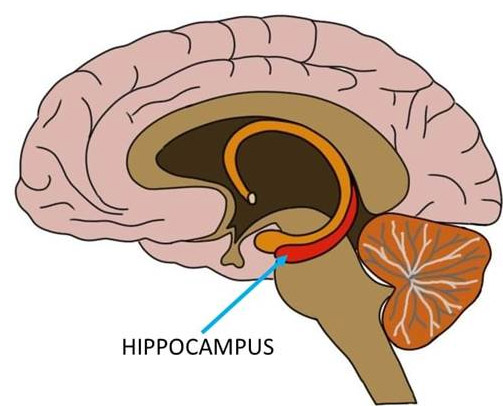
Several animal models have examined the relationship between occlusion, mastication and cognitive function. Using a mouse model, young animals fed a soft diet demonstrated reduced cognitive ability compared to young animals fed hard chow. There was a reduction in spatial memory. Histologically, there was a reduction in the number of nerve cells, nerve activity and new nerve growth in the hippocampus in animals fed a soft diet. The hippocampus is a bilateral part of the brain located behind the frontal lobe, in front of the occipital lobe and above the ventricles (see Figure 1). This is one of the first parts of the brain to demonstrate damage in AD7Fukushima-Nakayama Y, et al. Reduced mastication impairs memory function. J Dent Res. 2017;96(9):1058-66 https://www.ncbi.nlm.nih.gov/pubmed/28621563..
Another study utilized a mouse model specific for AD. These animals were genetically altered to over produce amyloid β (Aβ) protein. The accumulation of Aβ plaques in the brain has been closely associated with development of AD. Compared to animals of the same age that were not over producing Aβ, the experimental animals had reduced efficiency in mastication, and a lower biting force, but motor function was otherwise normal8Kim HB, et al. Abeta accumulation in vmo contributes to masticatory dysfunction in 5XFAD Mice. J Dent Res. 2021;100(9):960-7 https://www.ncbi.nlm.nih.gov/pubmed/33719684.. Histological analysis revealed Aβ accumulation in the trigeminal motor nucleus (cranial nerve 5, the trigeminal nerve, which controls biting as well as chewing function). The experimental mice also had smaller masseter muscles.
The two studies examine different aspects of the mastication/occlusion and cognitive function relationship. Neither study provides definitive proof of the temporal relationship between altered mastication and AD in humans, and they differ in the area of the brain that is affected. However, such animal studies support the need for clinical trials to examine the relationship in patients.
Cross-Sectional Clinical Studies:
Cross-sectional studies can identify an association between a proposed risk factor for a disease and development of that disease and are generally the first type of clinical study to be performed. Examining representative studies, they can be grouped by the focus of the impairment, here either reduced chewing capacity, or increased tooth loss, which would adversely affect mastication.
Examining chewing ability, an early report9Miura H, et al. Relationship between cognitive function and mastication in elderly females. J Oral Rehabil. 2003;30(8):808-11 https://www.ncbi.nlm.nih.gov/pubmed/12880404. evaluated women over 65 years of age. Half (N=44) were diagnosed with dementia, and an equal number did not demonstrate cognitive decline. Basic daily functions such as bathing and eating, cognitive decline, and masticatory/occlusal status, including the number of missing teeth and occlusal contacts, were assessed. Their simple conclusion: there was an association between reduced masticatory function and reduced cognitive function.
Other cross-sectional studies support this association and have elaborated and expanded on the earlier findings. A representative population study from Sweden included 557 older adults 77 years of age and older who were evaluated for cognitive function and provided a self-assessment of their dental status and chewing comfort10Lexomboon D, et al. Chewing ability and tooth loss: association with cognitive impairment in an elderly population study. J Am Geriatr Soc. 2012;60(10):1951-6 https://www.ncbi.nlm.nih.gov/pubmed/23035667.. Participants with significant tooth loss and difficulty masticating hard food were at greater risk of having cognitive impairment. Of note, having prosthetic replacement of missing teeth was not associated with cognitive impairment if the person did not report difficulty chewing. Similar findings supporting the importance of chewing efficiency vs. the number of teeth has been reported by others11Elsig F, et al. Tooth loss, chewing efficiency and cognitive impairment in geriatric patients. Gerodontology. 2015;32(2):149-56 https://www.ncbi.nlm.nih.gov/pubmed/24128078.. This study determined chewing efficiency by the mixing of a two-color paste. Evaluating a rural population of older adults in South Korea, chewing ability was again associated with an increased risk for reduced cognitive function12Kim EK, et al. Relationship between chewing ability and cognitive impairment in the rural elderly. Arch Gerontol Geriatr. 2017;70:209-13 https://www.ncbi.nlm.nih.gov/pubmed/28214402.. This finding was confirmed in a later study also from South Korea13Kim MS, et al. The association between mastication and mild cognitive impairment in Korean adults. Medicine (Baltimore). 2020;99(23):e20653 https://www.ncbi.nlm.nih.gov/pubmed/32502052..
Another report found that a reduced number of teeth and/or functional occlusal units was/were directly related to cognitive impairment14Cardoso MG, et al. Relationship between functional masticatory units and cognitive impairment in elderly persons. J Oral Rehabil. 2019;46(5):417-23 https://www.ncbi.nlm.nih.gov/pubmed/30614023.. A similar study reported that having fewer occluding units was also associated with eating a diet that contained more soft food15Popovac A, et al. Oral health status and nutritional habits as predictors for developing alzheimer's disease. Med Princ Pract. 2021;30(5):448-54 https://www.ncbi.nlm.nih.gov/pubmed/34348313.. Persons with dementia have also been reported to have a less balanced posterior occlusion16Park T, et al. More teeth and posterior balanced occlusion are a key determinant for cognitive function in the elderly. Int J Environ Res Public Health. 2021;18(4) https://www.ncbi.nlm.nih.gov/pubmed/33669490..
Analyzing the relationship between tooth loss and cognitive function, the relationship between the volume of grey matter in the brain and tooth loss was evaluated17Lin CS, et al. Association between tooth loss and gray matter volume in cognitive impairment. Brain Imaging Behav. 2020;14(2):396-407 https://www.ncbi.nlm.nih.gov/pubmed/32170642.. Grey matter is a major structural part of the central nervous system and differs from white matter in having more nerve cell bodies and fewer myelinated axons. Patients with mild cognitive impairment were compared to cognitively normal controls. Both groups received magnetic resonance imaging, as well as evaluation of oral status, including the number of teeth and masticatory function. Analyzing the relationship of volume of grey matter to oral findings, they reported:
- Controlling for other variables better masticatory function was associated with a greater volume of grey matter in the controls.
- For those with cognitive impairment, as the number of missing teeth increased, the volume of grey matter decreased.
- Among other locations, changes were most pronounced in the hippocampus, specifically in the left side temporal lobe.
Here the focus was on tooth loss as the risk factor.
A few studies have examined both tooth loss and chewing ability as risk factors for cognitive impairment. A study of 300 individuals compared the results of the standardized Mini-Mental State Examination (SMMSE). All participants displayed some degree of cognitive impairment18Kumar S, et al. Oral health status and treatment need in geriatric patients with different degrees of cognitive impairment and dementia: a cross-sectional study. J Family Med Prim Care. 2021;10(6):2171-6 https://www.ncbi.nlm.nih.gov/pubmed/34322409.. Both the total number of teeth lost, and poor mastication, were significantly associated with lower SMMSE scores. It is important to note that not all published studies have found this association. A similar study used the SMMSE to assess cognitive impairment did not report an association of cognitive impairment with poor mastication or tooth loss19Delwel S, et al. Chewing efficiency, global cognitive functioning, and dentition: A cross-sectional observational study in older people with mild cognitive impairment or mild to moderate dementia. Front Aging Neurosci. 2020;12:225 https://www.ncbi.nlm.nih.gov/pubmed/33033478..
Valuable information can also be obtained from data in national health surveys. Analyzing data available from Japan’s national healthcare system, people 65 years of age and older were evaluated for the relationship of cognitive impairment to the number of natural teeth20Da Silva JD, et al. Association between cognitive health and masticatory conditions: a descriptive study of the national database of the universal healthcare system in Japan. Aging (Albany NY). 2021;13(6):7943-52 https://www.ncbi.nlm.nih.gov/pubmed/33739304.. There were more than 33,000,000 records in the database, and comparison was made between those with and without cognitive impairment. Using a variety of patterns of tooth loss, persons with impaired mastication were more likely to display cognitive impairment (odds ratio of 1.89 for ‘early’ elderly and 1.33 for ‘late’ elderly, both p<0.0001). ‘Early’ elderly who were edentulous had an odds ratio of 2.38, while ‘late’ elderly had an odds ratio of 1.38. Using U.S. national health data, representing more than 100,000 individuals, an association between loss of teeth and cognitive impairment has also been reported21Galindo-Moreno P, et al. The impact of tooth loss on cognitive function. Clin Oral Investig. 2022;26(4):3493-500 https://www.ncbi.nlm.nih.gov/pubmed/34881401.. Of importance, a gradient was present, such that as tooth loss increased, so did the risk of cognitive impairment.
Longitudinal Clinical Studies:
While cross-sectional studies examining if a potential risk factor (here reduced masticatory function and/or tooth loss) is related to a disease (cognitive impairment) can provide evidence of a relationship, such studies only report a single time point. Potential confounding variables can be considered, but the temporal relationship of the risk factor to the disease (presence, progression) cannot be determined. Therefore, longitudinal studies offer a more informative approach. However, the logistics of a longitudinal study are far more challenging, including both design, analysis and cost.
A limited number of longitudinal studies have examined the relationship of mastication and tooth loss to cognitive impairment, and the results are supportive of the expected association (as mastication was reduced, and/or tooth loss increased, greater cognitive impairment was observed).
An early report examined the participants in a study of aging, health and body status. All participants were between 70 and 79 years of age. During a 5-year period, the MMSE exam was administered in years 1, 3 and 5, and a periodontal exam was performed in year 2. A close cross-sectional association between poor periodontal health and cognitive decline was seen. After controlling for many potential confounders, including age and education, only gingival inflammation was seen as a predictor of cognitive decline22Stewart R, et al. Adverse oral health and cognitive decline: The health, aging and body composition study. J Am Geriatr Soc. 2013;61(2):177-84 https://www.ncbi.nlm.nih.gov/pubmed/23405916..
More recently, 544 Swedish adults 50 years of age and older were followed for as long as 22 years to determine the relationship between specific cognitive functions such as verbal activity and perceptions, as well as dementia, and mastication as determined by the Eichner classification23Dintica CS, et al. The relation of poor mastication with cognition and dementia risk: A population-based longitudinal study. Aging (Albany NY). 2020;12(9):8536-48 https://www.ncbi.nlm.nih.gov/pubmed/32353829.. This scheme is based on occluding posterior teeth, with group A having contacts in all 4 posterior sextants, group B in 1-3 sextants and group C having none. Over time, participants in Eichner in categories B and C demonstrated greater decline in spatial aptitude. However, Eichner groups B and C did not demonstrate greater risk for dementia.
A 10 year South Korean study evaluated the relationship of chewing efficacy to cognitive function24Kim MS, Han DH. Does reduced chewing ability efficiency influence cognitive function? Results of a 10-year national cohort study. Medicine (Baltimore). 2022;101(25):e29270 https://www.ncbi.nlm.nih.gov/pubmed/35758356.,25Ko KA, et al. The Impact of Masticatory Function on Cognitive Impairment in Older Patients: A Population-Based Matched Case-Control Study. Yonsei Med J. 2022;63(8):783-9 https://www.ncbi.nlm.nih.gov/pubmed/35914761.. There were more than 10,000 participants at baseline, and those that were available were examined every 2 years for dementia (the MMSE) and chewing efficiency. After controlling for potential confounding variables, reduced chewing function was associated with a 28% increase in the risk for dementia. The authors concluded by noting the need to provide oral health care to individuals with poor mastication as an approach to prevention of cognitive decline.
Another study from South Korea examined the same question. Two groups were established: individuals with dementia (N=122) and controls (N=366). The two evaluations were conducted at baseline between 2005 and 2010, and the follow-up between 2014 and 2020, with an average period of observation of 9 years. The groups were established after the second evaluation. At baseline, none of the participants demonstrated dementia. Examining a range of potential oral disease risk factors over time, for the dementia group the number of “total functional tooth units” decreased, which was not seen in the control group. They also evaluated the number of teeth extracted, and rehabilitation of missing teeth. The analysis revealed that the number of missing teeth that were not restored (odd ratio = 1.195) and a history of alcohol consumption (odds ration = 4.445) were the most important risk factors for dementia(25). The authors suggested an associated between missing posterior teeth that were not restored, and dementia.
Conclusions Drawn in Review Papers
The interest in the relationship of mastication to cognitive function, as evidenced by the number of published studies, indicates the potential significance of this association, and suggests potential preventive and treatment approaches. These approaches could be employed to address the growing number of older adults that are and will be affected by cognitive impairment and dementia26Garre-Olmo J. [Epidemiology of Alzheimer's disease and other dementias]. Rev Neurol. 2018;66(11):377-86 https://www.ncbi.nlm.nih.gov/pubmed/29790571.,27Stephan BCM, et al. Secular Trends in Dementia Prevalence and Incidence Worldwide: A Systematic Review. J Alzheimers Dis. 2018;66(2):653-80 https://www.ncbi.nlm.nih.gov/pubmed/30347617.,28Lopez OL, Kuller LH. Epidemiology of aging and associated cognitive disorders: Prevalence and incidence of Alzheimer's disease and other dementias. Handb Clin Neurol. 2019;167:139-48 https://www.ncbi.nlm.nih.gov/pubmed/31753130.. Over the past 10-15 years, review papers have provided an overview of this area of investigation.
A number of these reviews have focused on the area of the brain that is affected by a reduction in mastication. In both animal models and human studies, the focus is on the hippocampus, considered the location for memory and learning. Hippocampus activity is reduced with aging29Ono Y, et al. Occlusion and brain function: mastication as a prevention of cognitive dysfunction. J Oral Rehabil. 2010;37(8):624-40 https://www.ncbi.nlm.nih.gov/pubmed/20236235.,30Kubo KY, et al. Masticatory function and cognitive function. Okajimas Folia Anat Jpn. 2010;87(3):135-40 https://www.ncbi.nlm.nih.gov/pubmed/21174943.,31Chen H, et al. Chewing Maintains Hippocampus-Dependent Cognitive Function. Int J Med Sci. 2015;12(6):502-9 https://www.ncbi.nlm.nih.gov/pubmed/26078711.. A linkage to chronic stress has also been suggested, as limited ability to chew will restrict the diet. Stress is associated with an increase in corticosteroid production, which is associated with increased risk of progression of disease, including cognition32Azuma K, et al. Association between Mastication, the Hippocampus, and the HPA Axis: A Comprehensive Review. Int J Mol Sci. 2017;18(8) https://www.ncbi.nlm.nih.gov/pubmed/28771175.. Another review focused on the frontotemporal cortex (including the hippocampus) as well as other parts of the brain, including the nucleus of the trigeminal nerve33Chuhuaicura P, et al. Mastication as a protective factor of the cognitive decline in adults: A qualitative systematic review. Int Dent J. 2019;69(5):334-40 https://www.ncbi.nlm.nih.gov/pubmed/31140598.,34Lopez-Chaichio L, et al. Oral health and healthy chewing for healthy cognitive ageing: A comprehensive narrative review. Gerodontology. 2021;38(2):126-35 https://www.ncbi.nlm.nih.gov/pubmed/33179281.. The direct benefit of proper occlusion is increased perfusion (blood flow) to those areas of the brain, with release of stimulatory mediators and prevention of β-amyloid plaque formation.
Clinically, reviews support the association of poor mastication and cognitive decline34Lopez-Chaichio L, et al. Oral health and healthy chewing for healthy cognitive ageing: A comprehensive narrative review. Gerodontology. 2021;38(2):126-35 https://www.ncbi.nlm.nih.gov/pubmed/33179281.,35Tada A, Miura H. Association between mastication and cognitive status: A systematic review. Arch Gerontol Geriatr. 2017;70:44-53 https://www.ncbi.nlm.nih.gov/pubmed/28042986.. In terms of the sequalae of tooth loss, restoration with a proper-functioning prosthesis serves to ameliorate the adverse effect of tooth loss that would result in limited mastication36Ahmed SE, et al. Influence of Dental Prostheses on Cognitive Functioning in Elderly Population: A Systematic Review. J Pharm Bioallied Sci. 2021;13(Suppl 1):S788-S94 https://www.ncbi.nlm.nih.gov/pubmed/34447202.. However, not all authors that reviewed the available literature concluded that extensive tooth loss is a risk factor for cognitive decline. Additional studies, with proper design, were felt to be needed37Tonsekar PP, et al. Periodontal disease, tooth loss and dementia: Is there a link? A systematic review. Gerodontology. 2017;34(2):151-63 https://www.ncbi.nlm.nih.gov/pubmed/28168759..
Other reviews remind us that there is a converse effect that may be important. Cognitive impairment can lead to an affected individual neglecting their oral health, not performing routine oral hygiene procedures and not accessing regular professional dental care38Nangle MR, Manchery N. Can chronic oral inflammation and masticatory dysfunction contribute to cognitive impairment? Curr Opin Psychiatry. 2020;33(2):156-62 https://www.ncbi.nlm.nih.gov/pubmed/31895157.,39Nakamura T, et al. Oral dysfunctions and cognitive impairment/dementia. J Neurosci Res. 2021;99(2):518-28 https://www.ncbi.nlm.nih.gov/pubmed/33164225.. Therefore, this relationship is an important consideration in determining cause and effect40Weijenberg RAF, et al. Mind your teeth-The relationship between mastication and cognition. Gerodontology. 2019;36(1):2-7 https://www.ncbi.nlm.nih.gov/pubmed/30480331.. The heterogenous nature of the evidence linking poor mastication to cognitive decline, without a consistent methodology41Asher S, et al. Periodontal health, cognitive decline, and dementia: A systematic review and meta-analysis of longitudinal studies. J Am Geriatr Soc. 2022;70(9):2695-709 https://www.ncbi.nlm.nih.gov/pubmed/36073186., indicates that specific criteria are needed for future studies, including prospective trial design that follows patients over time, consideration of a broad range of potentially confounding variables such as behavioral analysis, with a goal of determining the “effect size” of masticatory dysfunction on cognitive impairment42Lin CS. Revisiting the link between cognitive decline and masticatory dysfunction. BMC Geriatr. 2018;18(1):5 https://www.ncbi.nlm.nih.gov/pubmed/29304748..
Final Comments
This essay has provided an overview of the relationship of altered mastication to cognitive impairment. As is the case for many chronic diseases, dementia and AD are complex disorders that result from the influence of many risk factors. Genetics, weight, diet, socioeconomic factors are among these recognized risk factors43Wu YT, et al. The changing prevalence and incidence of dementia over time - current evidence. Nat Rev Neurol. 2017;13(6):327-39 https://www.ncbi.nlm.nih.gov/pubmed/28497805.. There is no single, primary etiological factor, and no primary means of prevention. Nevertheless, the body of evidence suggests a linkage between oral disease and cognitive decline, both from the standpoint of etiology (the role of the periodontal pathogen P. gingivalis), as well as the importance of maintenance of normal occlusion, and the effect of tooth loss and reduced masticatory capacity.
Oral health care providers must be aware of the expanding body of information linking oral disease/oral dysfunction to certain chronic diseases, here tooth loss, altered occlusion, and reduced mastication adversely affecting cognitive function. Discussing these topics with dental patients should focus on what is known. Maintenance of a functional, healthy dentition, which begins early in life, is to be emphasized. Restoring a dentition affected by tooth loss certainly improves oral health quality of life and may also have additional benefits that both reduce the risk for certain chronic diseases, and thereby improve general health.
References
- 1.Dominy SS, et al. Porphyromonas gingivalis in Alzheimer's disease brains: Evidence for disease causation and treatment with small-molecule inhibitors. Sci Adv. 2019;5(1):eaau3333 https://www.ncbi.nlm.nih.gov/pubmed/30746447.
- 2.Sadrameli M, et al. Linking mechanisms of periodontitis to Alzheimer's disease. Curr Opin Neurol. 2020;33(2):230-8 https://www.ncbi.nlm.nih.gov/pubmed/32097126.
- 3.Borsa L, et al. Analysis the link between periodontal diseases and Alzheimer's disease: A systematic review. Int J Environ Res Public Health. 2021;18(17) https://www.ncbi.nlm.nih.gov/pubmed/34501899.
- 4.Costa MJF, et al. Relationship of Porphyromonas gingivalis and Alzheimer's disease: A systematic review of pre-clinical studies. Clin Oral Investig. 2021;25(3):797-806 https://www.ncbi.nlm.nih.gov/pubmed/33469718.
- 5.Munoz Fernandez SS, Lima Ribeiro SM. Nutrition and Alzheimer disease. Clin Geriatr Med. 2018;34(4):677-97 https://www.ncbi.nlm.nih.gov/pubmed/30336995.
- 6.Aquilani R, et al. Is the Brain Undernourished in Alzheimer's Disease? Nutrients. 2022;14(9) https://www.ncbi.nlm.nih.gov/pubmed/35565839.
- 7.Fukushima-Nakayama Y, et al. Reduced mastication impairs memory function. J Dent Res. 2017;96(9):1058-66 https://www.ncbi.nlm.nih.gov/pubmed/28621563.
- 8.Kim HB, et al. Abeta accumulation in vmo contributes to masticatory dysfunction in 5XFAD Mice. J Dent Res. 2021;100(9):960-7 https://www.ncbi.nlm.nih.gov/pubmed/33719684.
- 9.Miura H, et al. Relationship between cognitive function and mastication in elderly females. J Oral Rehabil. 2003;30(8):808-11 https://www.ncbi.nlm.nih.gov/pubmed/12880404.
- 10.Lexomboon D, et al. Chewing ability and tooth loss: association with cognitive impairment in an elderly population study. J Am Geriatr Soc. 2012;60(10):1951-6 https://www.ncbi.nlm.nih.gov/pubmed/23035667.
- 11.Elsig F, et al. Tooth loss, chewing efficiency and cognitive impairment in geriatric patients. Gerodontology. 2015;32(2):149-56 https://www.ncbi.nlm.nih.gov/pubmed/24128078.
- 12.Kim EK, et al. Relationship between chewing ability and cognitive impairment in the rural elderly. Arch Gerontol Geriatr. 2017;70:209-13 https://www.ncbi.nlm.nih.gov/pubmed/28214402.
- 13.Kim MS, et al. The association between mastication and mild cognitive impairment in Korean adults. Medicine (Baltimore). 2020;99(23):e20653 https://www.ncbi.nlm.nih.gov/pubmed/32502052.
- 14.Cardoso MG, et al. Relationship between functional masticatory units and cognitive impairment in elderly persons. J Oral Rehabil. 2019;46(5):417-23 https://www.ncbi.nlm.nih.gov/pubmed/30614023.
- 15.Popovac A, et al. Oral health status and nutritional habits as predictors for developing alzheimer's disease. Med Princ Pract. 2021;30(5):448-54 https://www.ncbi.nlm.nih.gov/pubmed/34348313.
- 16.Park T, et al. More teeth and posterior balanced occlusion are a key determinant for cognitive function in the elderly. Int J Environ Res Public Health. 2021;18(4) https://www.ncbi.nlm.nih.gov/pubmed/33669490.
- 17.Lin CS, et al. Association between tooth loss and gray matter volume in cognitive impairment. Brain Imaging Behav. 2020;14(2):396-407 https://www.ncbi.nlm.nih.gov/pubmed/32170642.
- 18.Kumar S, et al. Oral health status and treatment need in geriatric patients with different degrees of cognitive impairment and dementia: a cross-sectional study. J Family Med Prim Care. 2021;10(6):2171-6 https://www.ncbi.nlm.nih.gov/pubmed/34322409.
- 19.Delwel S, et al. Chewing efficiency, global cognitive functioning, and dentition: A cross-sectional observational study in older people with mild cognitive impairment or mild to moderate dementia. Front Aging Neurosci. 2020;12:225 https://www.ncbi.nlm.nih.gov/pubmed/33033478.
- 20.Da Silva JD, et al. Association between cognitive health and masticatory conditions: a descriptive study of the national database of the universal healthcare system in Japan. Aging (Albany NY). 2021;13(6):7943-52 https://www.ncbi.nlm.nih.gov/pubmed/33739304.
- 21.Galindo-Moreno P, et al. The impact of tooth loss on cognitive function. Clin Oral Investig. 2022;26(4):3493-500 https://www.ncbi.nlm.nih.gov/pubmed/34881401.
- 22.Stewart R, et al. Adverse oral health and cognitive decline: The health, aging and body composition study. J Am Geriatr Soc. 2013;61(2):177-84 https://www.ncbi.nlm.nih.gov/pubmed/23405916.
- 23.Dintica CS, et al. The relation of poor mastication with cognition and dementia risk: A population-based longitudinal study. Aging (Albany NY). 2020;12(9):8536-48 https://www.ncbi.nlm.nih.gov/pubmed/32353829.
- 24.Kim MS, Han DH. Does reduced chewing ability efficiency influence cognitive function? Results of a 10-year national cohort study. Medicine (Baltimore). 2022;101(25):e29270 https://www.ncbi.nlm.nih.gov/pubmed/35758356.
- 25.Ko KA, et al. The Impact of Masticatory Function on Cognitive Impairment in Older Patients: A Population-Based Matched Case-Control Study. Yonsei Med J. 2022;63(8):783-9 https://www.ncbi.nlm.nih.gov/pubmed/35914761.
- 26.Garre-Olmo J. [Epidemiology of Alzheimer's disease and other dementias]. Rev Neurol. 2018;66(11):377-86 https://www.ncbi.nlm.nih.gov/pubmed/29790571.
- 27.Stephan BCM, et al. Secular Trends in Dementia Prevalence and Incidence Worldwide: A Systematic Review. J Alzheimers Dis. 2018;66(2):653-80 https://www.ncbi.nlm.nih.gov/pubmed/30347617.
- 28.Lopez OL, Kuller LH. Epidemiology of aging and associated cognitive disorders: Prevalence and incidence of Alzheimer's disease and other dementias. Handb Clin Neurol. 2019;167:139-48 https://www.ncbi.nlm.nih.gov/pubmed/31753130.
- 29.Ono Y, et al. Occlusion and brain function: mastication as a prevention of cognitive dysfunction. J Oral Rehabil. 2010;37(8):624-40 https://www.ncbi.nlm.nih.gov/pubmed/20236235.
- 30.Kubo KY, et al. Masticatory function and cognitive function. Okajimas Folia Anat Jpn. 2010;87(3):135-40 https://www.ncbi.nlm.nih.gov/pubmed/21174943.
- 31.Chen H, et al. Chewing Maintains Hippocampus-Dependent Cognitive Function. Int J Med Sci. 2015;12(6):502-9 https://www.ncbi.nlm.nih.gov/pubmed/26078711.
- 32.Azuma K, et al. Association between Mastication, the Hippocampus, and the HPA Axis: A Comprehensive Review. Int J Mol Sci. 2017;18(8) https://www.ncbi.nlm.nih.gov/pubmed/28771175.
- 33.Chuhuaicura P, et al. Mastication as a protective factor of the cognitive decline in adults: A qualitative systematic review. Int Dent J. 2019;69(5):334-40 https://www.ncbi.nlm.nih.gov/pubmed/31140598.
- 34.Lopez-Chaichio L, et al. Oral health and healthy chewing for healthy cognitive ageing: A comprehensive narrative review. Gerodontology. 2021;38(2):126-35 https://www.ncbi.nlm.nih.gov/pubmed/33179281.
- 35.Tada A, Miura H. Association between mastication and cognitive status: A systematic review. Arch Gerontol Geriatr. 2017;70:44-53 https://www.ncbi.nlm.nih.gov/pubmed/28042986.
- 36.Ahmed SE, et al. Influence of Dental Prostheses on Cognitive Functioning in Elderly Population: A Systematic Review. J Pharm Bioallied Sci. 2021;13(Suppl 1):S788-S94 https://www.ncbi.nlm.nih.gov/pubmed/34447202.
- 37.Tonsekar PP, et al. Periodontal disease, tooth loss and dementia: Is there a link? A systematic review. Gerodontology. 2017;34(2):151-63 https://www.ncbi.nlm.nih.gov/pubmed/28168759.
- 38.Nangle MR, Manchery N. Can chronic oral inflammation and masticatory dysfunction contribute to cognitive impairment? Curr Opin Psychiatry. 2020;33(2):156-62 https://www.ncbi.nlm.nih.gov/pubmed/31895157.
- 39.Nakamura T, et al. Oral dysfunctions and cognitive impairment/dementia. J Neurosci Res. 2021;99(2):518-28 https://www.ncbi.nlm.nih.gov/pubmed/33164225.
- 40.Weijenberg RAF, et al. Mind your teeth-The relationship between mastication and cognition. Gerodontology. 2019;36(1):2-7 https://www.ncbi.nlm.nih.gov/pubmed/30480331.
- 41.Asher S, et al. Periodontal health, cognitive decline, and dementia: A systematic review and meta-analysis of longitudinal studies. J Am Geriatr Soc. 2022;70(9):2695-709 https://www.ncbi.nlm.nih.gov/pubmed/36073186.
- 42.Lin CS. Revisiting the link between cognitive decline and masticatory dysfunction. BMC Geriatr. 2018;18(1):5 https://www.ncbi.nlm.nih.gov/pubmed/29304748.
- 43.Wu YT, et al. The changing prevalence and incidence of dementia over time - current evidence. Nat Rev Neurol. 2017;13(6):327-39 https://www.ncbi.nlm.nih.gov/pubmed/28497805.